Warburg and Krebs and related effects in cancer
Published online by Cambridge University Press: 27 September 2019
Abstract
Warburg and coworkers' observation of altered glucose metabolism in tumours has been neglected for several decades, which, in part, was because of an initial misinterpretation of the basis of their finding. Following the realisation that genetic alterations are often linked to metabolism, and that the tumour micro-environment imposes different demands on cancer cells, has led to a reinvestigation of cancer metabolism in recent years. Increasing our understanding of the drivers and consequences of the Warburg effect in cancer and beyond will help to identify new therapeutic strategies as well as to identify new prognostic and therapeutic biomarkers. Here we discuss the initial findings of Warburg and coworkers regarding cancer cell glucose metabolism, how these studies came into focus again in recent years following the discovery of metabolic oncogenes, and the therapeutic potential that lies within targeting the altered metabolic phenotype in cancer. In addition, another essential nutrient in cancer metabolism, glutamine, will be discussed.
초록
워버그와 동료들이 종양에서 변화된 포도당 대사 현상을 관찰한 것은
수십 년간 소홀히 다루어졌으며,
이는 부분적으로 그들의 발견의 기반에 대한 초기 오해 때문이었습니다.
유전적 변이가 대사 과정과 밀접하게 연관되어 있으며,
종양 미세환경이 암 세포에 다른 요구사항을 부과한다는 인식이 확산되면서
최근 몇 년간 암 대사 연구가 재검토되었습니다.
워버그 효과의 원인 및 암을 넘어 그 영향에 대한 이해를 심화시키는 것은
새로운 치료 전략을 식별하고 예후 및 치료 바이오마커를 발견하는 데 기여할 것입니다.
본 논문에서는
워버그와 동료들의 암 세포 포도당 대사 관련 초기 연구 결과,
대사 관련 암 유전자 발견 이후 최근 다시 주목받게 된 이 연구들의 배경,
그리고 암의 변형된 대사 형질을 표적으로 삼는 치료적 잠재력에 대해 논의합니다.
또한 암 대사에서 또 다른 필수 영양소인
글루타민에 대해서도 논의됩니다.
Introduction
The way cancer has been considered and investigated over the last century has been mainly as a genetic disease primarily characterised by dysregulated cell growth. A variety of aberrations in oncogenes leading to gain of function or amplification, and in tumour suppressor genes from inactivating point mutations or epigenetic silencing, have been considered as responsible for the cancer phenotype. Although this understanding has helped to unravel many aspects of this complex disease, it also led to the neglect of early, often biochemical findings, on the role of cancer metabolism, such as the Warburg effect. New evidence is now linking many tumour suppressors and oncogenes to the regulation of metabolism and the need of highly-proliferating cancer cells to juggle nutrient utilisation in a manner that supports continuous and fast cell growth and survival. In over two-third of human cancers, at least one glycolytic gene is constitutively overexpressed (Ref. Reference Altenberg and Greulich1). Thus, current research is actually returning back to classical biochemical studies to further understand their implication in disease initiation and progression with the hope that new applications of those old discoveries will lead to the development of new therapeutics.
Cancer cells, like highly proliferating normal cells, are faced with the task to generate sufficient ATP to maintain energy status as well to produce increasing amounts of biosynthetic metabolites and precursors, whilst balancing the cellular redox status. In particular, for cancer cells, they also need to adapt their metabolic processes to a different environment from normal tissue, where nutrient supplies may be exhausted as well as instability in the redox balance, pH and oxygen levels (Ref. Reference Muir and Vander Heiden2). One such adaptive mechanism is aerobic glycolysis or the Warburg effect, in which cancer cells ferment glucose to lactate despite an ample oxygen supply.
This review describes the Warburg effect from a historical perspective, how this fundamental finding on cancer metabolism was forgotten for several decades before re-emerging with the discovery of metabolic oncogenes and how the Warburg effect forms the basis of several therapeutic strategies in cancer currently used or in development.
서론
지난 세기 동안 암은 주로 유전적 질환으로 간주되어 왔으며, 주로 조절되지 않은 세포 증식으로 특징지어졌습니다.
종양 유전자(oncogenes)의 기능 획득 또는 증폭을 초래하는 다양한 이상과,
종양 억제 유전자(tumour suppressor genes)의 비활성화 점 돌연변이 또는
에피제네틱 침묵화 등이 암의 표현형에 책임이 있다고 여겨져 왔습니다.
이 이해는 이 복잡한 질병의 많은 측면을 밝히는 데 기여했지만,
암 대사 역할에 대한 초기 생화학적 발견,
예를 들어 워버그 효과와 같은 연구를 소홀히 하는 결과를 초래했습니다.
새로운 증거는
많은 종양 억제 유전자와 종양 유전자가 대사 조절과 고도로 증식하는 암 세포가
지속적인 빠른 세포 성장과 생존을 지원하기 위해
영양소 이용을 조절해야 하는 필요성과 연결되고 있습니다.
인간 암의 2/3 이상에서 적어도 하나의 글리코겐 분해 유전자가
지속적으로 과발현됩니다(참조: Reference Altenberg and Greulich1).
따라서 현재 연구는
질병 발병 및 진행에 대한 이해를 심화하기 위해 고전적인 생화학적 연구로 돌아가고 있으며,
이러한 오래된 발견의 새로운 응용이 새로운 치료법 개발로 이어질 것을 기대하고 있습니다.
암 세포는
고도로 증식하는 정상 세포와 마찬가지로 충분한 ATP를 생성하여 에너지 상태를 유지하고
생합성 대사산물 및 전구체를 증가시키며,
동시에 세포 내 산화환원 상태를 균형 있게 유지해야 합니다.
특히 암 세포는 정상 조직과 다른 환경에 적응해야 하며,
이 환경에서는 영양소 공급이 고갈될 수 있으며
산화환원 균형, pH 및 산소 수준이 불안정할 수 있습니다(Ref. Reference Muir and Vander Heiden2).
이러한 적응 메커니즘 중 하나가
유산소 당분해 또는 워버그 효과로,
암 세포는 충분한 산소 공급에도 불구하고 포도당을 젖산으로 발효합니다.
이 리뷰는 워버그 효과를 역사적 관점에서 설명하며,
이 암 대사 연구의 근본적 발견이 대사 종양 유전자 발견으로 재발견되기 전
수십 년간 잊혀졌던 과정을 조명합니다.
또한
워버그 효과가 현재 사용 중이거나 개발 중인
여러 암 치료 전략의 기반을 형성하는 방식을 설명합니다.
Historical perspectives on the Warburg effect
Warburg's work on glycolysis in cancer cells came at a time when the scientific community was mainly focusing on lipolysis and/or proteolysis as the energy-providing reactions that drive cancer cell growth rather than on glucose metabolism (Ref. Reference Warburg3). Following on from his observations on the sea urchin egg, for which a significant increase in oxygen uptake and rapid cell division occurred after fertilisation, Warburg expected a similar increase in oxygen uptake in cancer tissues (Refs Reference Warburg3, Reference Warburg4).
Together with Seigo Minami, Warburg observed that Flexner–Jobling rat liver tumours were able to acidify the surrounding isotonic salt solution after the addition of glucose by releasing lactic acid into this solution (Ref. Reference Warburg and Minami5). Warburg and coworkers went on to further examine glycolysis in rat liver carcinoma slices by measuring oxygen consumption as well as carbon dioxide production under aerobic and anaerobic settings using his improved manometric technique (Refs Reference Warburg, Posener and Negelein6, Reference Warburg7). In this experimental set up, they made three key observations: (1) the production of lactic acid under anaerobic conditions was much higher in rat carcinoma tissues compared with the reference values from the literature for, for example, human blood or frog muscle, (2) the carcinoma did not take up more oxygen under aerobic conditions than normal tissue and (3) by moving the carcinoma from anaerobic to aerobic conditions, the amount of lactate produced was only marginally reduced (Ref. Reference Warburg, Posener and Negelein6). These findings can be summarised as aerobic glycolysis or later termed the Warburg effect, which is the preference of tumours for fermentation of glucose to lactate even in the presence of sufficient amounts of oxygen. This is in contrast to normal tissue that exhibits the Pasteur effect of completely stopping lactate production in the presence of sufficient amounts of oxygen (Fig. 1) (Ref. Reference Warburg, Posener and Negelein6). Similar results were obtained in different human carcinomas (from larynx, intestine, penis, nose and skin) and comparison with benign tumours showed that malignant tissue produced 3–4 times more lactic acid (Ref. Reference Warburg, Posener and Negelein6). Elegant in vivo experiments by Cori and Cori demonstrated that low lactic acid concentrations within the tumour were maintained by releasing lactic acid into the bloodstream (Refs Reference Cori and Cori8, Reference Cori and Cori9). Later experiments by Warburg and coworkers revealed even higher levels of fermentation in Ehrlich ascites cancer cells from mice compared with the findings in rat sarcomas, a fact probably because of a higher percentage of cancer cells in the mouse ascites cancer (Ref. Reference Warburg and Ernst10).
워버그 효과의 역사적 관점
워버그의 암 세포에서의 글리코lysis 연구는 과학계가 주로 암 세포 성장의 에너지 공급 반응으로 리포lysis와/또는 프로테olysis에 초점을 맞추고 있었을 때 진행되었습니다. 글루코스 대사(Ref. Reference Warburg3)보다는 말이죠. 워버그는 해삼 알에 대한 관찰 결과, 수정 후 산소 섭취량이 크게 증가하고 세포 분열이 급속히 진행되는 현상을 바탕으로, 암 조직에서도 유사한 산소 섭취량 증가를 예상했습니다(참조 Reference Warburg3, Reference Warburg4).
세이고 미나미와 함께 워버그는 Flexner–Jobling 쥐 간 종양이 포도당을 추가한 후 이 용액에 젖산을 방출하여 주변 등장액 염용액을 산성화할 수 있음을 관찰했습니다(Ref. Reference Warburg and Minami5). 워버그와 동료들은 개선된 만계측 기술을 사용하여 쥐 간 암 조직 슬라이스에서 산소 소비량과 이산화탄소 생산량을 산소 존재 조건과 무산소 조건에서 측정함으로써 글리코lysis를 추가로 조사했습니다(참고문헌 Reference Warburg, Posener and Negelein6, Reference Warburg7). 이 실험 설정에서 그들은 세 가지 주요 관찰 결과를 얻었습니다:
(1) 무산소 조건에서 쥐 암 조직의 젖산 생산량은 문헌상의 참고 값(예: 인간 혈액이나 개구리 근육)과 비교해 훨씬 높았으며,
(2) 암 조직은 산소 조건에서 정상 조직보다 더 많은 산소를 섭취하지 않았으며,
(3) 암 조직을 무산소 조건에서 산소 조건으로 이동시켰을 때 생성된 젖산 양은 약간만 감소했습니다(Ref. 참고 문헌 Warburg, Posener 및 Negelein6).
이러한 결과는 산소 조건에서도 포도당을 젖산으로 발효시키는 종양의 선호 현상인 '호기성 당분해' 또는 나중에 '워버그 효과'로 요약될 수 있습니다.
이는 정상 조직이 충분한 산소 조건에서 젖산 생산을 완전히 중단하는 '파스퇴르 효과'와 대조됩니다(그림 1) (참조: Warburg, Posener 및 Negelein6). 인간 암종(후두, 장, 음경, 코, 피부)에서 유사한 결과가 얻어졌으며, 양성 종양과의 비교에서 악성 조직은 3~4배 더 많은 젖산을 생성했습니다(Ref. Reference Warburg, Posener and Negelein6). Cori와 Cori의 우아한 in vivo 실험은 종양 내 낮은 젖산 농도가 혈류로 젖산을 방출함으로써 유지된다는 것을 보여주었습니다(참조 Cori와 Cori8, Cori와 Cori9). Warburg와 동료들의 후속 실험은 쥐의 Ehrlich 복수 암 세포에서 쥐 사르코마에서 관찰된 것보다 훨씬 높은 발효 수준을 보여주었으며, 이는 쥐 복수 암에서 암 세포의 비율이 더 높기 때문일 가능성이 높습니다(Ref. Reference Warburg and Ernst10).
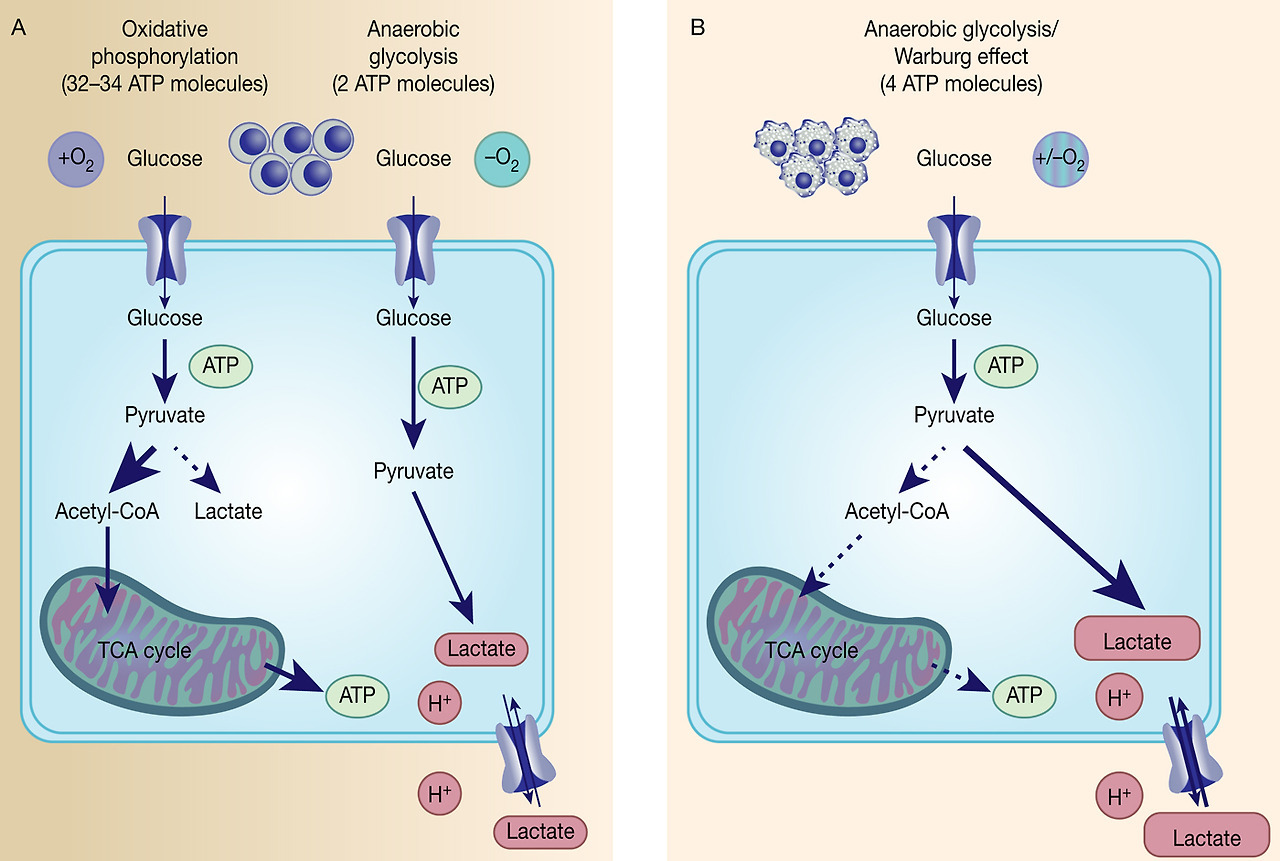
Fig. 1. The Warburg effect in cancer. Differentiated, normal tissues (a) metabolise glucose depending on oxygen levels with normoxic conditions favouring complete glucose metabolism in the mitochondria to maximise ATP production (oxidative phosphorylation). Under low oxygen levels, the majority of glucose will be metabolised to lactate, which is excreted from the cells, but allows sustaining a minimum level of ATP production (anaerobic glycolysis). In contrast, tumour cells (b) mainly metabolise glucose to lactate independent from intracellular oxygen levels and despite of thereby producing less ATP compared with full oxidation of pyruvate within the mitochondria (aerobic glycolysis or Warburg effect).
그림 1. 암에서의 워버그 효과. 분화된 정상 조직(a)은 산소 농도에 따라 포도당을 대사하며, 정상 산소 조건에서는 미토콘드리아에서 포도당 대사(산화적 인산화)가 완전히 이루어져 ATP 생산을 최대화합니다. 산소 농도가 낮은 조건에서는 대부분의 포도당이 젖산으로 대사되어 세포 밖으로 배출되지만, 최소 수준의 ATP 생산을 유지합니다(무산소성 당분해). 반면, 암 세포(b)는 세포 내 산소 농도와 무관하게 주로 포도당을 젖산으로 대사하며, 이는 미토콘드리아 내 피루브산의 완전 산화(호기성 당분해)에 비해 ATP 생산량이 적습니다(무산소성 당분해 또는 워버그 효과).
Warburg initially reasoned that the observed decrease in oxidative phosphorylation under normoxic conditions was because of defects in the mitochondrial respiration of cancer cells resulting in compromised aerobic respiration and subsequent reliance on glycolytic metabolism (Ref. Reference Warburg11). To him the irreversible injury of respiration was the essential common cause and origin of cancer, a hypothesis that led to major scientific controversies and was generally not accepted among most biochemists and oncologists because of missing experimental evidence (Refs Reference Warburg12, Reference Weinhouse13, Reference Racker and Spector14). However, subsequent evidence emerged to suggest that respiration is generally not impaired in cancer cells and today we appreciate that the high rate of glycolysis exhibited by cancer cells under normoxic conditions is not due to damaged respiration, but rather changes in the molecular aspects of glycolysis.
However, the reasons behind the Warburg effect are under continuous investigation. Although oxidative phosphorylation yields between 32 and 34 ATP molecules per molecule of glucose, glycolysis only produces two molecules of ATP per molecule of glucose (Ref. Reference Cooper15) (Fig. 1). Despite being the energetically less favourable pathway, it is likely that there is a selective advantage for cancer cells to adapt their metabolism to glycolysis, such as being a way to balance energy production and generation of necessary building blocks to support proliferation.
워버그는 초기 연구에서 정상 산소 조건 하에서 관찰된 산화적 인산화 감소가 암 세포의 미토콘드리아 호흡 결함으로 인해 산소 호흡이 손상되고 이후 당분해 대사 의존으로 이어지기 때문이라고 추론했습니다(참조 Reference Warburg11). 그에게 호흡의 불가역적 손상은 암의 필수적인 공통 원인과 기원으로, 이 가설은 실험적 증거 부족으로 인해 대부분의 생화학자와 종양학자 사이에서 받아들여지지 않았으며 주요 과학적 논쟁을 일으켰습니다(참조 Reference Warburg12, Reference Weinhouse13, Reference Racker and Spector14). 그러나 후속 증거는 암 세포에서 호흡이 일반적으로 손상되지 않았음을 보여주었으며, 오늘날 우리는 암 세포가 정상 산소 조건 하에서 높은 글리코겐 분해 속도를 보이는 것이 호흡 손상 때문이 아니라 글리코겐 분해의 분자적 측면 변화 때문임을 이해하게 되었습니다.
그러나 워버그 효과의 원인은 계속 연구 중입니다. 산화적 인산화(oxidative phosphorylation)는 글루코스 분자당 32~34개의 ATP 분자를 생성하지만, 글리코lysis는 글루코스 분자당 2개의 ATP 분자만을 생성합니다(Ref. Reference Cooper15) (Fig. 1). 에너지 효율이 낮은 경로임에도 불구하고, 암 세포가 에너지 생산과 증식을 지원하기 위한 필수 구성 요소 생성을 균형 있게 조절하는 방법으로서 글리코lysis로 대사 경로를 적응시키는 선택적 이점이 있을 가능성이 있습니다.
Rediscovery of the metabolic role in cancer through the Darwinian evolution of the cancer genome
Over the last two decades, there has been a strongly increasing interest and re-examination of the Warburg effect and cancer metabolism with the reprogramming of metabolism in cancer being added to the original set of hallmarks of cancer from Hanahan and Weinberg in 2011 (Ref. Reference Hanahan and Weinberg16).
Prior cancer research had mainly focused on understanding genetic alterations in cancer with the identification of oncogenes and tumour suppressor genes as main types of cancer-causing genes (Refs Reference Stehelin17, Reference Tabin18), while oncogenic alterations of cell metabolism were considered as secondary effects. Extensive studies of the genetics of many tumours, facilitated by high-throughput sequencing techniques, highlight the strong inter- and intratumour heterogeneity, which account for one of the major challenges in the treatment of cancer. Our current understanding of how intratumour genetic complexity arises follows one of the first descriptions of cancer as an evolutionary process from Peter Nowell in the 1970s (Ref. Reference Nowell19). Reminiscent of the Darwinian evolution theory of the ‘survival of the fittest’, tumourigenesis follows a natural selection process governed by environmental selection forces and cellular adaption strategies in order to confer a selective survival advantage to the cell (Refs Reference Nowell19, Reference Greaves20). This perception had not only brought the importance of the tumour micro-environment back into focus, but also made researchers look more closely at how cancer cells adapt to the particular challenges of a highly proliferative cell, and thus cancer metabolism. Additionally, further elucidation of cancer-related driver mutations, that is, mutations that arise during tumourigenesis and provide a selective advantage for the tumour cells, identified that many have a significant role in core signalling pathways responsible for nutrient uptake and metabolism (Ref. Reference Sever and Brugge21). It has been shown that many mutated key signalling pathways come together in order to adapt tumour metabolism and to sustain tumour growth and survival (Ref. Reference Sever and Brugge21).
Historically, the first metabolic pathways to be studied biochemically in cancer were the nucleotide de novo and salvage pathways. Enhanced activities of enzymes within these pathways, especially of the salvage pathway, leading to increased nucleotide levels were reported in tumours, such as hepatomas, lung and renal cell carcinoma (Refs Reference Jackson22, Reference Natsumeda23). Increased nucleotide synthesis in cancer epitomises the adaption of metabolism to cope with the demands of high proliferation and has been a consistent area of interest and target for chemotherapeutics (see ‘Antimetabolites’). Although alterations in nucleotide metabolism have been studied continuously, carbohydrate metabolism, the focus of this review, went through a long period of neglect. It was only after the identification of germline mutations in different metabolic enzymes, such as fumarate hydratase (FH), succinate dehydrogenase (SDH) and isocitrate dehydrogenase (IDH), that metabolic enzymes involved in this pathway were considered to play an important role in tumourigenesis (Refs Reference Tomlinson24–Reference Parsons26). Today, not only are mutations in oncogenes or tumour suppressor genes known to impact on metabolic reprogramming, but also the idea of metabolic oncogenes has emerged, such as highlighted in the cases of IDH and 3-phosphoglycerate dehydrogenase (PHGDH).
암의 대사적 역할 재발견: 암 유전체 진화를 통한 다윈주의적 접근
지난 20년간 암의 대사 재프로그래밍이 2011년 Hanahan과 Weinberg가 제시한 암의 주요 특징에 추가되면서 워버그 효과와 암 대사 연구에 대한 관심과 재검토가 급증했습니다(참조: Reference Hanahan and Weinberg16).
이전 암 연구는 주로 암의 유전적 변이를 이해하는 데 초점을 맞췄으며, 암 유발 유전자로 온코겐과 종양 억제 유전자가 주요 유형으로 식별되었습니다(참조 Stehelin17, Tabin18). 반면 세포 대사 과정의 암 유발 변이는 부차적 효과로 간주되었습니다. 고속 시퀀싱 기술로 가능해진 많은 종양의 유전학 연구는 종양 내외의 강한 이질성을 강조하며, 이는 암 치료의 주요 도전 과제 중 하나입니다. 현재 종양 내 유전적 복잡성이 어떻게 발생하는지에 대한 이해는 1970년대 Peter Nowell이 암을 진화 과정으로 처음 설명한 내용(Ref. Reference Nowell19)을 따르고 있습니다. 다윈의 자연 선택 이론인 '적자 생존'과 유사하게, 종양 발생은 환경적 선택 압력과 세포적 적응 전략에 의해 지배되는 자연 선택 과정을 통해 세포에 선택적 생존 우위를 부여합니다(참조 Reference Nowell19, Reference Greaves20). 이 인식은 종양 미세환경의 중요성을 다시 한 번 강조했을 뿐만 아니라, 암 세포가 고도로 증식하는 세포의 특정한 도전 과제에 어떻게 적응하는지, 그리고 따라서 암 대사 과정에 더 주목하게 만들었습니다. 또한 암 관련 드라이버 돌연변이, 즉 종양 발생 과정에서 발생하여 종양 세포에 선택적 우위를 제공하는 돌연변이의 추가적인 규명은 많은 돌연변이가 영양소 흡수 및 대사 담당 핵심 신호 전달 경로에 중요한 역할을 한다는 것을 밝혀냈습니다(Ref. Reference Sever and Brugge21). 많은 변이된 핵심 신호 전달 경로가 종양 대사 적응과 종양 성장 및 생존을 유지하기 위해 함께 작용한다는 것이 입증되었습니다(Ref. Reference Sever and Brugge21).
역사적으로 암에서 생화학적 연구로 처음 조사된 대사 경로는 뉴클레오티드 신생합성 및 재활용 경로입니다. 이러한 경로 내 효소의 활성 증가, 특히 재활용 경로의 활성 증가로 인해 뉴클레오티드 수치가 증가한다는 보고가 암종(간암, 폐암, 신세포암 등)에서 확인되었습니다(Ref. Reference Jackson22, Reference Natsumeda23). 암에서의 뉴클레오티드 합성 증가 는 높은 증식 요구에 대응하기 위한 대사 적응을 상징하며, 화학요법의 주요 관심 분야이자 표적이 되어 왔습니다('항대사물질' 참조). 그러나 뉴클레오티드 대사 변화가 지속적으로 연구되어 왔음에도 불구하고, 이 리뷰의 초점인 탄수화물 대사는 오랜 기간 소홀히 되었습니다. 다양한 대사 효소(예: 푸마레이트 하이드라타제(FH), 수크신산 탈수소효소(SDH), 이소시트르산 탈수소효소(IDH))의 유전적 변이가 발견된 후, 이 경로에 관여하는 대사 효소가 종양 발생에 중요한 역할을 한다는 것이 인정되기 시작했습니다(참고문헌 Tomlinson24–Parsons26). 현재는 종양 유전자나 종양 억제 유전자의 변이가 대사 재프로그래밍에 영향을 미친다는 것이 알려져 있을 뿐만 아니라, IDH와 3-포스포글리세레이트 탈수소효소(PHGDH) 사례에서 강조된 것처럼 대사 종양 유전자의 개념이 등장했습니다.
IDH1/2 as an example in malignant gliomas/AML
Identification of somatic activating mutations in IDH1 in glioblastoma (GBM) was a key to opening a renewed interest in cancer metabolism and its impact on tumourigenesis (Ref. Reference Parsons26). IDH1 encodes a cytosolic form of IDH, which catalyses the oxidative carboxylation of isocitrate to α-ketoglutarate (α-KG) within the Krebs cycle. A large sequence analysis of 20 661 protein coding genes in 22 human tumour samples identified point mutations in IDH1 which all lead to substitutions in the same amino acid (arginine 132) and were mainly prevalent in younger patients (mean age of 33 years) and patients with secondary GBM (Ref. Reference Parsons26). Initial follow-up studies found mutations in IDH1 or IDH2 in over 70% of WHO grade II/III astrocytomas, oligodendrogliomas and GBMs (Ref. Reference Yan27) as well as IDH1 mutations in about 8% of acute myeloid leukaemia (AML) patient samples (Ref. Reference Mardis28) with later genomic analysis confirming IDH mutations in several types of cancer (reviewed in Ref. Reference Dang, Yen and Attar29).
Both IDH1 and IDH2 mutations cause a gain-of-function in enzyme activity towards reduction of α-KG to the oncometabolite R-2-hydroxyglutarate (2-HG) while oxidising NADPH/H+ (Refs Reference Dang30, Reference Ward31). Although 2-HG is only present at very low concentrations in normal cells with no attributed function (Ref. Reference Dang, Yen and Attar29), it was not clear how 2-HG was potentially driving cancer. The first hint came from a profiling study of DNA methylation patterns in GBM tumours in which a large subset (mainly from the proneural subtype) displayed a hypermethylation pattern of CpG islands (CIMP) together with a frequent IDH1 mutation (Ref. Reference Noushmehr32). This correlation between the CIMP phenotype and IDH1 mutation was further strengthened by showing that the introduction of a mutation in IDH1 was sufficient to establish the hypermethylator phenotype in gliomas (Ref. Reference Turcan33). Mutational and epigenetic profiling of AML patients revealed IDH1/2 mutations to be mutually exclusive with loss-of-function mutations in TET2 (Ref. Reference Figueroa34). TET2 is an α-KG-dependent dioxygenase that hydrolyses 5-methylcytosine, and is one of several α-KG-dependent dioxygenase, including histone methyltransferases, histone demethylases and prolyl hydroxylases, that is competitively inhibited by 2-HG (Ref. Reference Xu35). Thus, a mutation in IDH1/IDH2 leads to the accumulation of the oncometabolite 2-HG which in turn then inhibits various α-KG-dependent dioxygenases resulting in a genome-wide alteration of the histone and DNA methylation pattern (Fig. 2).
IDH1/2를 악성 뇌종양/급성 골수성 백혈병(AML)의 예시로
IDH1의 체세포 활성화 돌연변이를 글리오blastoma (GBM)에서 식별하는 것은 암 대사 및 그 종양 발생에 미치는 영향에 대한 새로운 관심을 불러일으키는 데 핵심적인 역할을 했습니다 (참조: Reference Parsons26). IDH1은 Krebs 회로 내에서 이소시트르산을 α-케토글루타레이트 (α-KG)로 산화적 카복실화 반응을 촉매하는 세포질 형태의 IDH를编码합니다. 22개의 인간 종양 샘플에서 20,661개의 단백질 코딩 유전자를 대상으로 한 대규모 시퀀스 분석에서 IDH1의 점 돌연변이가 발견되었으며, 이는 모두 동일한 아미노산(아르기닌 132)의 대체를 초래했으며, 주로 젊은 환자(평균 연령 33세)와 2차성 GBM 환자에서 주로 관찰되었습니다(Ref. Reference Parsons26). 초기 추적 연구에서 WHO 등급 II/III 아스트로사이트종(astrocytomas)의 70% 이상, 올리고덴드로글리오마 및 GBM(Ref. Reference Yan27)에서 발견되었으며, 급성 골수성 백혈병(AML) 환자 샘플의 약 8%에서 IDH1 돌연변이가 확인되었습니다(Ref. Reference Mardis28). 후속 유전체 분석은 여러 유형의 암에서 IDH 돌연변이를 확인했으며(Ref. Reference Dang, Yen and Attar29에서 검토됨).
IDH1 및 IDH2 돌연변이는 α-KG를 암 대사산물 R-2-hydroxyglutarate (2-HG)로 환원시키는 효소 활성의 기능 획득을 유발하며, 동시에 NADPH/H+를 산화시킵니다(참조 문헌 Reference Dang30, Reference Ward31). 정상 세포에서는 2-HG가 매우 낮은 농도로 존재하며 기능이 알려지지 않았지만(Ref. Reference Dang, Yen and Attar29), 2-HG가 암을 촉진하는 메커니즘은 명확하지 않았습니다. 첫 번째 단서는 GBM 종양의 DNA 메틸화 패턴 프로파일링 연구에서 나왔습니다. 이 연구에서 주요 하위 유형(주로 proneural 하위 유형)을 포함한 대규모 하위 집합이 CpG 섬의 과메틸화 패턴(CIMP)과 함께 IDH1 돌연변이가 자주 관찰되었습니다(Ref. Reference Noushmehr32). CIMP 표현형과 IDH1 돌연변이의 상관관계는 IDH1 돌연변이를 도입하는 것만으로도 뇌종양에서 과메틸화 표현형을 유발할 수 있음을 보여줌으로써 더욱 강화되었습니다(Ref. Reference Turcan33). 급성 골수성 백혈병(AML) 환자의 돌연변이 및 에피게놈 프로파일링은 IDH1/2 돌연변이가 TET2의 기능 상실 돌연변이와 상호 배타적임을 보여주었습니다(Ref. Reference Figueroa34). TET2는 5-메틸시토신을 가수분해하는 α-KG 의존성 디옥시게나아제로, 히스톤 메틸전달효소, 히스톤 데메틸화효소 및 프로릴 하이드록시라제 등 여러 α-KG 의존성 디옥시게나아제 중 하나로, 2-HG에 의해 경쟁적으로 억제됩니다(Ref. Reference Xu35). 따라서 IDH1/IDH2의 돌연변이는 종양 대사산물 2-HG의 축적을 유발하며, 이는 다시 다양한 α-KG 의존성 디옥시게나제를 억제하여 히스톤 및 DNA 메틸화 패턴의 전장 유전체적 변화를 초래합니다(그림 2).
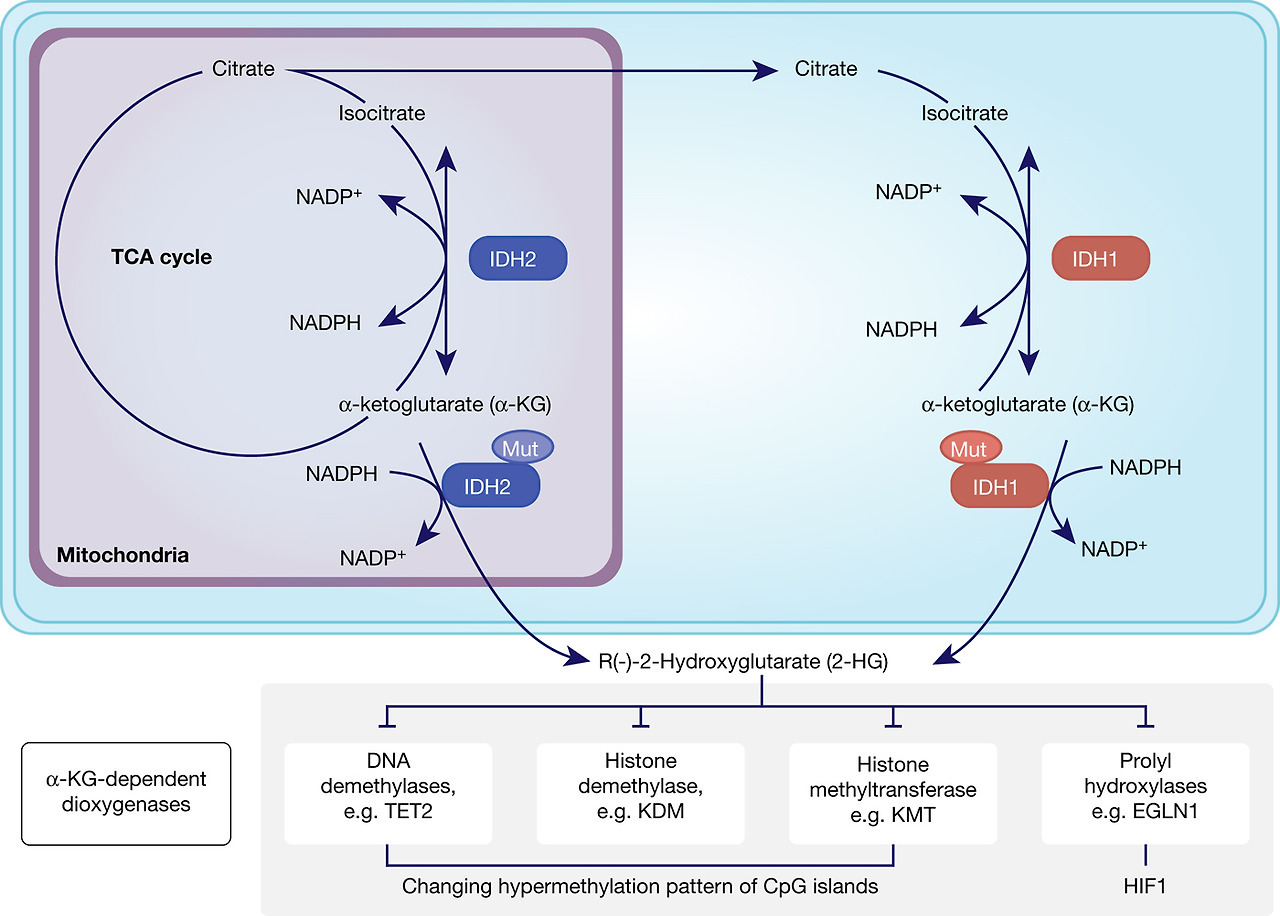
Fig. 2. Somatic IDH1/2 mutations reduce α-KG to the oncometabolite 2-HG. Mutant IDH1/2 (IDH1/2mut) have gained the function to reduce α-ketoglutarate (α-KG) to the oncometabolite R(-)-2-hydroxyglutarate either in the mitochondria by IDH2mut or in the cytosol by IDH1mut, which then inhibits several α-KG-dependent dioxygenases, which leads to genome-wide alteration of the histone and DNA-methylation patterns and HIF1 regulation.
그림 2. 체세포 IDH1/2 돌연변이는 α-KG를 종양 대사산물 2-HG로 감소시킵니다. 돌연변이 IDH1/2 (IDH1/2mut)는 미토콘드리아에서 IDH2mut에 의해 또는 세포질에서 IDH1mut에 의해 α-케토글루타르산 (α-KG)을 종양 대사산물 R(-)-2-하이드록시글루타르산으로 감소시키는 기능을 획득했습니다. 이는 α-KG에 의존하는 여러 디옥시게나아제의 활성을 억제하여 히스톤 및 DNA 메틸화 패턴의 전장 유전체적 변화와 HIF1 조절을 유발합니다.
However, the clear role of IDH mutations in tumour formation and progression is still being investigated. IDH1 mutations have been proposed as very early events in tumourigenesis in gliomas with IDH1 mutations occurring prior to the acquisition of TP53 mutations, loss of chromosome 1p/19q or copy number alterations of phosphatase and tensin homologue (PTEN) and EGFR (Refs Reference Watanabe36, Reference Lai37). IDH1 R132H mutation was also found to be the only shared mutation between initial and recurrent tumours of 23 GBM patients (Ref. Reference Johnson38) as well as being maintained in 95% of secondary GBMs in another analysed cohort of 106 gliomas (Ref. Reference Lass39). In addition, studies of haematopoietic disorders found IDH1/2 mutations in premalignant disease forms, such as myelodysplastic and myeloproliferative neoplasms (Refs Reference Kosmider40, Reference Pardanani41). However, in vivo mouse models introducing IDH2 mutations showed that this mutation on its own was insufficient to drive leukemogenesis and rather had the role of a cooperative tumourigenic driver in AML (Refs Reference Kats42, Reference Chen43). Although no spontaneous tumour formation was observed after introduction of an IDH1 mutation in several cell types of the murine central nervous system, mutant IDH1 seems to have a clear role in tumour maintenance as pharmacological inhibition of mutant IDH1 impairs growth in established glioma xenograft models (Refs Reference Sasaki44, Reference Rohle45). Although these findings support the role of IDH mutations in tumourigenesis and tumour maintenance, further investigations are needed to determine exactly to what extent and in what precise context.
그러나 IDH 돌연변이가 종양 형성 및 진행에 미치는 명확한 역할은 여전히 연구 중입니다. IDH1 돌연변이는 글리오마에서 종양 발생의 매우 초기 단계로 제안되었으며, IDH1 돌연변이는 TP53 돌연변이, 1p/19q 염색체 상실 또는 인산화효소 및 텐신 동형체(PTEN) 및 EGFR의 복제 수 변이 획득 전에 발생합니다(참조 Reference Watanabe36, Reference Lai37). IDH1 R132H 돌연변이는 23명의 GBM 환자의 초기 및 재발 종양에서 유일한 공통 돌연변이로 확인되었으며(Ref. Reference Johnson38), 다른 분석된 106개 뇌종양 코호트에서 2차 GBM의 95%에서 유지되었습니다(Ref. Reference Lass39). 또한 혈액 질환 연구에서 IDH1/2 돌연변이가 골수이형성 증후군 및 골수증식성 종양과 같은 전암성 질환 형태에서 발견되었습니다(참고문헌 Reference Kosmider40, Reference Pardanani41). 그러나 IDH2 변이를 도입한 생체 내 마우스 모델에서 이 변이만으로는 백혈병 발생을 유발하기에 충분하지 않았으며, 오히려 급성 골수성 백혈병(AML)에서 협력적 종양 발생 촉진자로 역할을 하는 것으로 나타났습니다(참조 Kats42, Chen43). 마우스 중추 신경계 여러 세포 유형에 IDH1 변이를 도입한 후 자연적인 종양 형성이 관찰되지 않았지만, 변이된 IDH1은 종양 유지에 명확한 역할을 하는 것으로 보입니다. 약리학적 억제로 변이된 IDH1을 억제하면 확립된 뇌종양 이종 이식 모델에서 성장 장애가 발생합니다(참조 Reference Sasaki44, Reference Rohle45). 이러한 결과는 IDH 돌연변이가 종양 발생 및 유지에 역할을 한다는 것을 지지하지만, 정확히 어느 정도이며 어떤 구체적인 맥락에서 작용하는지 확인하기 위해 추가 연구가 필요합니다.
PHGDH: the first enzyme of the de novo serine synthesis pathway
The de novo serine synthesis pathway comprises a three-step reaction cascade from 3-phosphoglycerate to L-serine, consecutively catalysed by PHGDH, phosphoserine aminotransferase (PSAT) and phosphoserine phosphatase (PSPH) (Fig. 3). The first indication of serine synthesis pathway alterations in cancer came from studies by Davis et al., who had observed increased PHGDH activity in rat hepatoma cell lines in comparison to their corresponding normal host liver cells (Ref. Reference Davis, Fallon and Morris46). Subsequent studies by Snell and coworkers confirmed increased PHGDH activity in rat hepatomas, which was correlated with their growth rate, as well as in human colon carcinoma samples providing yet more evidence of PHGDH's link to tumour initiation and progression (Refs Reference Snell and Weber47, Reference Snell48).
PHGDH: 세린 신생합성 경로의 첫 번째 효소
세린 신생합성 경로는 3-포스포글리세레이트에서 L-세린으로 이어지는 세 단계 반응 연쇄로 구성되며, 이 과정은 PHGDH, 포스포세린 아미노트랜스퍼레이즈 (PSAT) 및 포스포세린 포스파타제 (PSPH)에 의해 순차적으로 촉매됩니다 (그림 3). 암에서 세린 합성 경로의 변화에 대한 첫 번째 증거는 Davis 등(Ref. Reference Davis, Fallon and Morris46)의 연구에서 나왔으며, 이들은 쥐 간암 세포주에서 정상 호스트 간 세포에 비해 PHGDH 활성이 증가했음을 관찰했습니다. Snell과 동료들의 후속 연구는 쥐 간암에서 PHGDH 활성 증가를 확인했으며, 이는 성장 속도와 관련이 있었으며, 인간 대장 암 샘플에서도 PHGDH와 종양 발생 및 진행 간의 연관성을 추가로 입증했습니다(Ref. Reference Snell and Weber47, Reference Snell48).
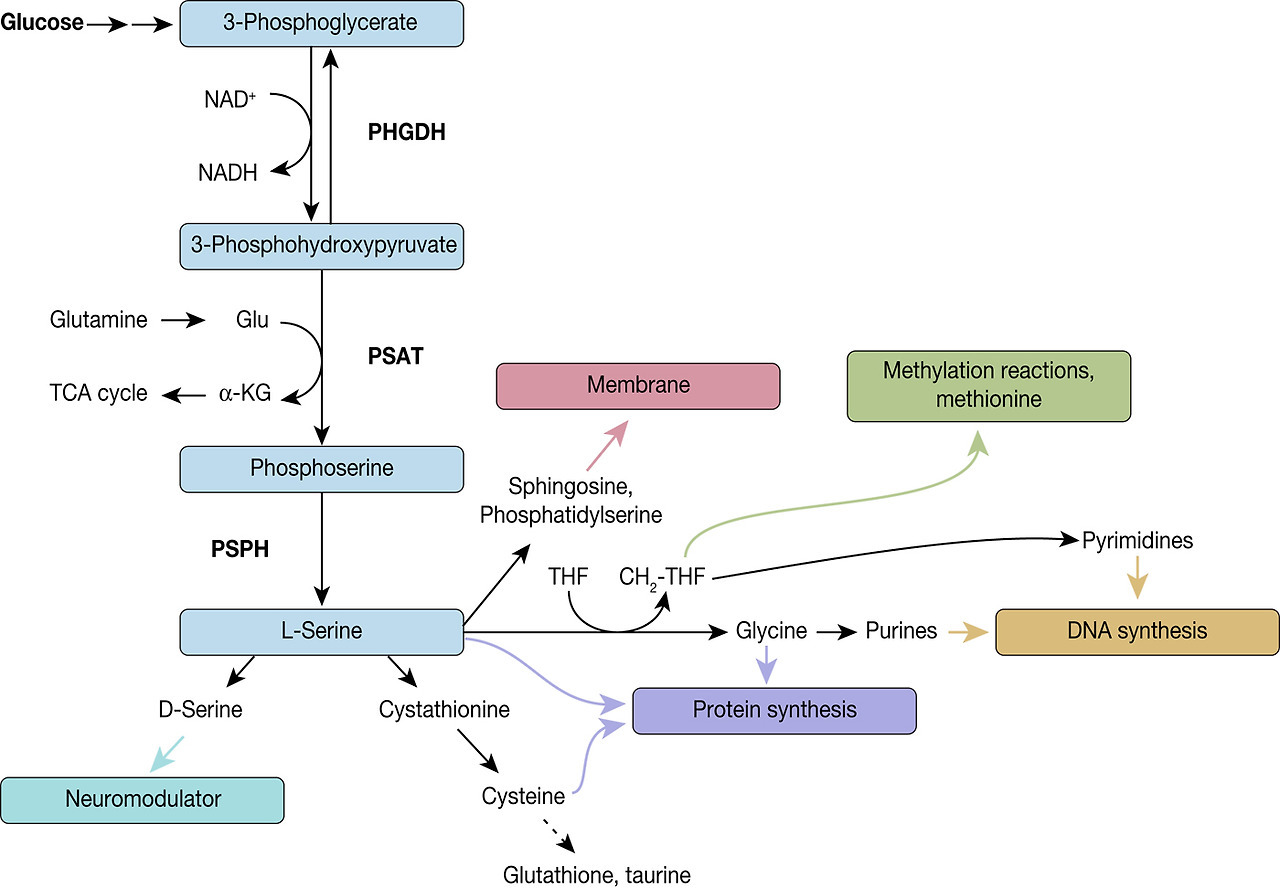
Fig. 3. Diversion into the synthesis of biomolecules through PHGDH. PHGDH diverts the glycolytic flux by oxidising 3-phosphoglycerate (3-PG) to 3-phosphohydroxypyruvate (3-PHP) and thereby reducing NAD+ to NADH. 3-PHP is further converted to phosphoserine by phosphoserine aminotransferase (PSAT), which is combined with the formation of α-ketoglutarate from glutamate, followed by dephosphorylation by phosphoserine phosphatase (PSPH) leading to L-serine. L-serine itself is a precursor for various biomolecules and by these means implicated in several biological processes, such as neuromodulation, protein and membrane synthesis, methylation reactions and DNA synthesis.
그림 3. PHGDH를 통해 생체분자 합성으로의 분기. PHGDH는 3-포스포글리세레이트 (3-PG)를 3-포스포히드록시피루베이트 (3-PHP)로 산화시켜 글리코lytic 흐름을 분기시키고, 이 과정에서 NAD+를 NADH로 환원시킵니다. 3-PHP는 인산세린 아미노트랜스퍼레이즈(PSAT)에 의해 인산세린으로 전환되며, 이는 글루타메이트로부터 α-케토글루타레이트의 형성 과정과 결합됩니다. 이후 인산세린 인산분해효소(PSPH)에 의해 인산분해되어 L-세린으로 전환됩니다. L-세린 자체는 다양한 생물분자의 전구체로 작용하며, 신경 조절, 단백질 및 막 합성, 메틸화 반응, DNA 합성 등 여러 생물학적 과정에 관여합니다.
However, only enzymatic activities had been compared so far and it was not until 25 years later that genomic and metabolomic analysis rediscovered PHGDH in the context of cancer (Refs Reference Locasale49–Reference Pollari51). Negative-selection RNAi screening in a human breast cancer xenograft model identified PHGDH within a predefined set of 133 metabolic enzymes as an essential gene for tumourigenesis and within a region of frequent copy number alterations (Ref. Reference Possemato50). Further analysis of a cohort of human breast tumours revealed 70% of ER-negative tumours having increased levels of PHGDH mRNA and protein (Ref. Reference Possemato50). This supported a previous study that had already shown a correlation between high PHGDH mRNA levels and poor 5-year survival in ER-negative, basal breast cancers (Ref. Reference Pollari51). Next to genomic amplification, PHGDH expression can also be upregulated by the transcription factors ATF4 (Ref. Reference Adams52) and c-Myc (Ref. Reference Nilsson53) or through epigenetic activation of PHGDH by histone H3 lysine 9 methyltransferase (Ref. Reference Ding54). In addition, reinvestigation of a pooled analysis of somatic copy number alterations revealed PHGDH as a frequently amplified gene across 3131 cancer samples (Ref. Reference Beroukhim55). PHGDH is located on chromosome 1p12 in a peak region that displays repeated copy number gain in 16% of the cancers assessed with no known oncogenes contained in that particular region (Refs Reference Locasale49, Reference Beroukhim55). The most common tumour type with PHGDH gain was melanoma, with 40% frequency in PHGDH amplification (Ref. Reference Beroukhim55). Consistent with the genetic data, reduced proliferation was seen in melanoma and breast cancer cell lines containing PHGDH copy number gain or elevated PHGDH expression following knockdown of PHGDH (Refs Reference Locasale49, Reference Possemato50). However, translation of these findings to xenograft models had different outcomes with studies in breast cancer and non-small cell lung cancer xenografts showing the suppression of tumour growth following PHGDH knockdown (Refs Reference Possemato50, Reference DeNicola56), whereas in another study no effect of PHGDH knockdown was observed in established breast cancer xenograft models (Ref. Reference Chen57).
To date, many tumour types have been reported to exhibit increased levels of PHGDH expression, such as cervical, glioma, colon, melanoma, pancreatic, liver as well as kidney tumours (Ref. Reference Grant58). However, how PHGDH drives tumourigenesis and progression still needs to be further validated. Overexpression of catalytic dead PHGDH fails to rescue the PHGDH knockdown phenotype (Ref. Reference Mattaini59), similarly, the supply of exogenous amounts of serine or methyl-serine-ester to the cell culture media does not restore cell proliferation following PHGDH knockdown (Ref. Reference Possemato50). Exploring a role for PHGDH beyond serine synthesis identified human PHGDH as being able to catalyse the NADH-dependent reduction of α-KG to the oncometabolite 2-HG, a function previously only known for PHGDH from Escherichia coli, but at the same time the amounts of 2-HG generated were 100–1000 times lower than those in IDH mutant cancers (Ref. Reference Fan60). Another study showed that hypoxia-induced HIF-1 and HIF-2 expression increased the expression of PHGDH and other enzymes of the de novo serine synthesis pathway, in breast cancer cell lines and breast cancer stem cells-enriched cell populations (Ref. Reference Samanta61). Under hypoxic conditions, PHGDH knockdown resulted in decreased NADPH levels and subsequent increase of mitochondrial ROS levels and sensitised breast cancer cell lines to carboplatin (Ref. Reference Samanta61). Additionally, PHGDH has been reported to stabilise the transcription factor FOXM1 in glioma, which in turn leads to increased expression of genes involved in tumour invasion, angiogenesis and cell cycle regulation (Ref. Reference Liu62). PHGDH has also been shown to be linked to the NAD+ salvage pathway with breast cancer cell lines overexpressing PHGDH being highly sensitive to inhibition of the NAD+ salvage pathway through NAMPT inhibitors (Ref. Reference Murphy63).
그러나 지금까지는 효소 활성만 비교되었을 뿐이며, 25년 후에야 유전체 및 대사체 분석을 통해 PHGDH가 암 맥락에서 재발견되었습니다(참고문헌 Reference Locasale49–Reference Pollari51). 인간 유방암 이종이식 모델에서 음성 선택 RNAi 스크리닝을 통해 PHGDH가 133개의 대사 효소 중 종양 발생에 필수적인 유전자로 식별되었으며, 이는 빈번한 복제 수 변이 지역 내에 위치했습니다(Ref. Reference Possemato50). 인간 유방 종양 코호트에 대한 추가 분석에서 ER 음성 종양의 70%에서 PHGDH mRNA 및 단백질 수준이 증가한 것으로 나타났습니다(Ref. Reference Possemato50). 이는 이전 연구에서 이미 ER 음성, 기저형 유방암에서 높은 PHGDH mRNA 수준과 5년 생존율 저하 사이의 상관관계를 보여준 결과를 뒷받침했습니다(Ref. Reference Pollari51). 유전체 증폭 외에도 PHGDH 발현은 전사 인자 ATF4(Ref. Reference Adams52) 및 c-Myc(Ref. Reference Nilsson53)에 의해 상향 조절되거나, 히스톤 H3 라이신 9 메틸트랜스퍼레이즈(Ref. Reference Ding54)에 의한 PHGDH의 에피제네틱 활성화로 인해 증가할 수 있습니다. 또한, 체세포 복제 수 변이 통합 분석의 재검토 결과, PHGDH는 3,131개의 암 샘플에서 자주 증폭된 유전자로 확인되었습니다(Ref. Reference Beroukhim55). PHGDH는 1p12 염색체에 위치하며, 해당 지역은 16%의 암에서 반복적인 복제 수 증가를 보이는 피크 지역이며, 해당 지역에는 알려진 종양 유전자가 포함되어 있지 않습니다(Ref. Reference Locasale49, Reference Beroukhim55). PHGDH 복제 수 증가가 가장 흔한 종양 유형은 흑색종으로, PHGDH 증폭 빈도는 40%였습니다(Ref. Reference Beroukhim55). 유전적 데이터와 일치하게, PHGDH 복제수 증가 또는 PHGDH 발현이 증가한 멜라노마 및 유방암 세포주에서 PHGDH 발현 억제 후 증식 감소가 관찰되었습니다(참조 Reference Locasale49, Reference Possemato50). 그러나 이러한 결과를 이종 이식 모델로 전환한 연구에서는 유방암과 비소세포 폐암 이종 이식 모델에서 PHGDH 발현 억제 후 종양 성장 억제가 관찰되었으나(Ref. Reference Possemato50, Reference DeNicola56), 다른 연구에서는 확립된 유방암 이종 이식 모델에서 PHGDH 발현 억제의 효과가 관찰되지 않았습니다(Ref. Reference Chen57).
현재까지 자궁경부암, 뇌종양, 대장암, 흑색종, 췌장암, 간암 및 신장암 등 다양한 종양 유형에서 PHGDH 발현 수준이 증가했다는 보고가 있습니다(Ref. Reference Grant58). 그러나 PHGDH가 종양 발생 및 진행을 어떻게 촉진하는지는 추가적인 검증が必要です. 촉매 활성이 없는 PHGDH의 과발현은 PHGDH 발현 억제 현상을 회복시키지 못했습니다(Ref. Reference Mattaini59). 마찬가지로, 세포 배양 매체에 세린 또는 메틸-세린 에스터를 외부에서 공급해도 PHGDH 발현 억제 후 세포 증식이 회복되지 않았습니다(Ref. Reference Possemato50). 세린 합성 beyond에서의 PHGDH의 역할을 탐구하는 과정에서 인간 PHGDH가 NADH 의존적 α-KG 환원 반응을 촉매하여 종양 대사산물 2-HG를 생성한다는 것이 밝혀졌습니다. 이 기능은 이전에는 Escherichia coli의 PHGDH에서만 알려져 있었지만, 동시에 생성된 2-HG의 양은 IDH 돌연변이 암에서 관찰된 양보다 100~1,000배 낮았습니다(Ref. Reference Fan60). 또 다른 연구에서는 저산소 조건에서 HIF-1 및 HIF-2 발현이 증가하여 유방암 세포주 및 유방암 줄기세포 풍부 세포군에서 PHGDH 및 세린 신합성 경로의 다른 효소 발현이 증가함을 보여주었습니다(Ref. Reference Samanta61). 저산소 조건에서 PHGDH 발현을 억제하면 NADPH 수준이 감소하고 미토콘드리아 ROS 수준이 증가하며, 이는 유방암 세포주에 카보플라틴에 대한 감수성을 높였습니다(Ref. Reference Samanta61). 또한 PHGDH는 뇌종양에서 전사 인자 FOXM1을 안정화시켜 종양 침윤, 혈관新生 및 세포 주기 조절과 관련된 유전자 발현을 증가시키는 것으로 보고되었습니다(Ref. Reference Liu62). PHGDH는 NAD+ 회수 경로와 연관되어 있으며, PHGDH 과발현 유방암 세포주는 NAMPT 억제제를 통해 NAD+ 회수 경로가 억제될 때 높은 감수성을 보였습니다(Ref. Reference Murphy63).
Oncogenes and tumour suppressors change the metabolic gene expression underlying aerobic glycolysis
In addition to the genetic mutations of metabolic enzymes, there are also other changes in molecular mechanisms that have been shown to contribute to the Warburg phenotype in cancer, such as activation of transcription factors (e.g. HIF-1 or Myc) or signalling pathways (e.g. PI3K/Akt) as well as the inactivation of tumour suppressors (e.g. p53). These genetic alterations have an impact on several aspects of cancer metabolism, but within the scope of this review, we will be focusing on mechanisms related to aerobic glycolysis.
온코진과 종양 억제 유전자는 유산소 당분해의 기초가 되는 대사 유전자 발현을 변화시킵니다
대사 효소의 유전적 변이 외에도, 암에서 워버그 현상에 기여하는 것으로 알려진 분자 메커니즘의 다른 변화들이 존재합니다. 예를 들어, 전사 인자(예: HIF-1 또는 Myc)의 활성화나 신호 전달 경로(예: PI3K/Akt)의 활성화, 종양 억제인자(예: p53)의 비활성화 등이 포함됩니다. 이러한 유전적 변이는 암 대사 과정의 여러 측면에 영향을 미치지만, 본 리뷰에서는 호기성 당분해와 관련된 메커니즘에 초점을 맞출 것입니다.
Activation of transcription factors
Amplified or overexpressed MYC has been identified in a plethora of human cancers and it was shown to transcriptionally regulate a variety of processes, such as proliferation, cell size, apoptosis and metabolism (Ref. Reference Meyer and Penn64). Following activation, c-Myc and its cofactor Max bind to the ‘E-boxes’ consensus sequences present in a majority of target genes involved in metabolism (Ref. Reference Kim65). Using 13C-labelled glucose, Myc has been shown to upregulate glucose consumption in Burkitt lymphoma cells (Ref. Reference Le66). Myc expression promotes glucose uptake through increasing the expression of glucose transporter GLUT1 as well as upregulating glucose catabolism through increased expression of glycolytic enzymes, such as hexokinase 2, phosphofructokinase-M 1 and enolase 1 (Refs Reference Kim65, Reference Osthus67). In addition, Myc was shown to block the transcription factor MondoA in triple-negative breast cancer, which results in the inhibition of thioredoxin-interacting protein to then stimulate aerobic glycolysis (Ref. Reference Shen68). Myc also upregulates the transcription of heterogeneous nuclear ribonucleoproteins and thereby indirectly promotes the expression of isoform M2 of pyruvate kinase (PKM2), which is the predominant isoform in cancer, supporting the diversion of glycolytic intermediates towards anabolic metabolism (Ref. Reference David69). The metabolic switch in cancer is further favoured by c-Myc-mediated activation of the enzymes within the de novo serine synthesis pathway, with PSPH being particularly important for c-Myc-driven hepatocellular cancer progression in vitro and in vivo (Ref. Reference Sun70). Another glycolytic gene upregulated by Myc is Lactate dehydrogenase A (LDHA), with lactate dehydrogenase A being responsible for the final step in aerobic glycolysis: the conversion of pyruvate to L-lactate (Ref. Reference Shim71). In addition, Myc also induces overexpression of the bidirectional monocarboxylate transporter MCT1, which facilitates lactate excretion from the cells (Ref. Reference Doherty72). Lactate has been proposed to support cancer aggressiveness by triggering angiogenesis and was shown to stimulate the accumulation of hypoxia-inducible factor 1 α (HIF-1α) activation in GBM cells (Refs Reference Sonveaux73, Reference Lu, Forbes and Verma74).
HIF-1 and HIF-2 are major transcription factors made of the heterodimeric complex of α and β subunits and responsible for the adaptive response to hypoxic conditions (Ref. Reference Maxwell, Pugh and Ratcliffe75). HIF1α is better characterised with regards to cancer metabolism. Under normoxic conditions, HIF1α levels are tightly regulated, but become aberrantly activated by oncogenic signalling pathways, such as PI3K/AKT/mTOR (Ref. Reference Sun76), or mutations in tumour suppressor proteins, such as the von Hippel–Lindau protein (VHL) (Ref. Reference Maxwell77). Independent of oxygen level mutations in the Krebs cycle, enzymes FH and SDH lead to overexpression and stabilisation of HIF1α by fumarate and succinate suggesting a positive feedback mechanism as HIF1α in turn promotes glycolysis (Refs Reference Gimenez-Roqueplo78, Reference Pollard79). Similar to Myc, glucose transporters as well as glycolytic enzymes are also under the control of HIF-1 and promote glucose import and glycolysis under normoxic conditions (Refs Reference Maxwell80, Reference Semenza81). In addition, HIF-1 also prevents the flux of pyruvate into the mitochondrial TCA cycle by activating pyruvate dehydrogenase kinase 1 (PDK1) as well as LDHA (Refs Reference Semenza81, Reference Kim82). PDK1 phosphorylates and thereby inactivates pyruvate dehydrogenase (PDH) and thus prevents the conversion of pyruvate to acetyl coenzyme A, the metabolite to enter mitochondrial TCA, while increased LDHA expression results in more pyruvate being metabolised to lactate.
Overall these activated transcription factors contribute to the reprogramming of the glucose metabolism according to Warburg's observations by: (1) promoting glucose uptake through upregulation of glucose transporters, (2) supporting aerobic glycolysis through increased expression of glycolytic enzymes under normoxic conditions and (3) supporting lactate production and excretion via monocarboxylate transporters (MCT) to divert pyruvate from the TCA cycle in the mitochondria (Fig. 4).
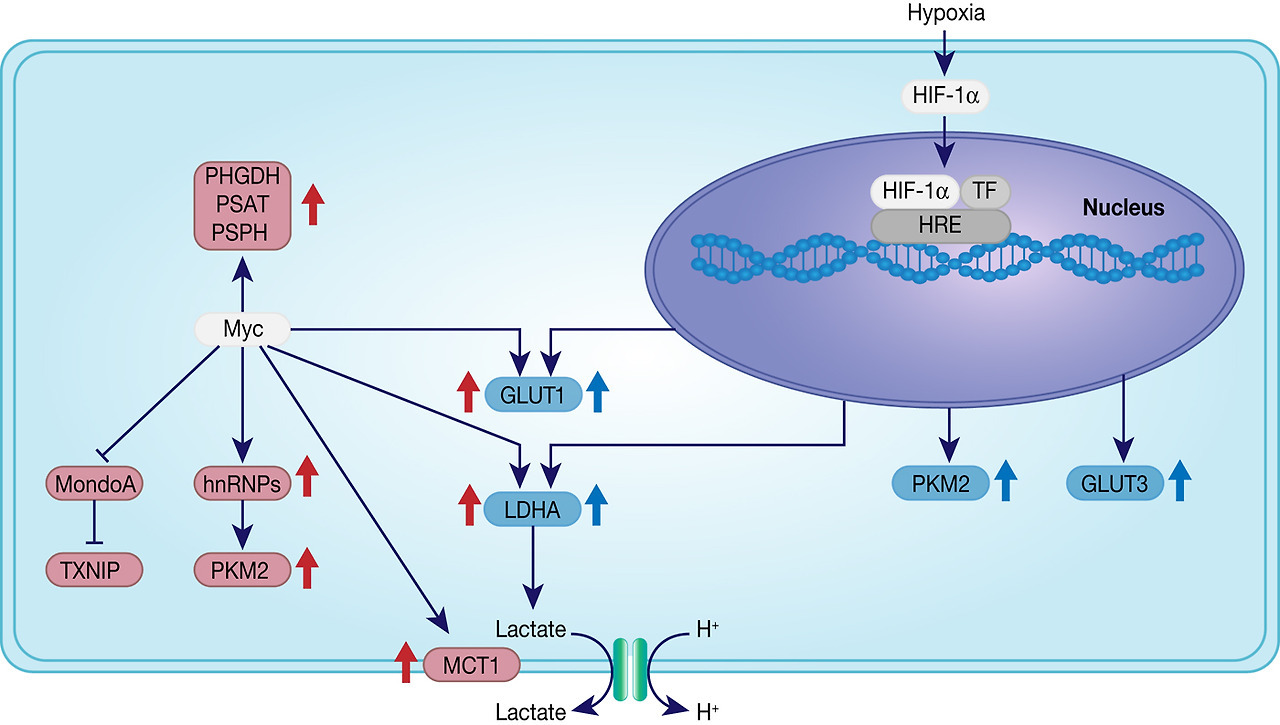
Fig. 4. Myc- and HIF1α-activated pathways. Myc and HIF1α promote the Warburg effect in cancer cells by upregulating critical pathways: increased glucose uptake through high expression of glucose transporters GLUT1 and GLUT3, increased lactate synthesis and excretion through overexpression of LDH-A and MCT1, diversion of the glycolytic metabolites to anabolic metabolism through upregulated PKM2, stimulation of aerobic glycolysis through inhibition of MondoA.
Inactivation of tumour suppressors: exemplified by p53
Several tumour suppressors have been reported to regulate cancer metabolism, such as PTEN and retinoblastoma protein as well as VHL, mentioned above (Ref. Reference Iurlaro, Leon-Annicchiarico and Munoz-Pinedo83). However, the most prominent representative of this group is p53 with missense mutations in its encoding gene TP53 occurring in up to 50% of all cancers (Ref. Reference Cole84). Loss of p53 function has been shown to contribute to the Warburg effect through several mechanisms. Glucose import into the cell is partly regulated by p53 through direct repression of the transcription of GLUT1 and GLUT4 as well as through inhibition of NF-κB, which represses GLUT3 expression (Refs Reference Schwartzenberg-Bar-Yoseph, Armoni and Karnieli85, Reference Kawauchi86). In addition, p53 induces the transcription of TIGAR (TP53-induced glycolysis and apoptosis regulator), which results in lowering the intracellular fructose-2,6-bisphosphate (F26BP) levels (Ref. Reference Bensaad87). As F26BP is the allosteric activator of phosphofructose kinase 1 (PFK1), its depletion decreases PFK1 activity and thus promotes diversion of glycolysis into the pentose phosphate pathway. P53 also intervenes with the conversion of pyruvate to lactate or acetyl-CoA by downregulating the monocarboxylate transporter MCT1 and thus lactate excretion from the cells on one hand whilst promoting conversion of pyruvate to acetyl-CoA by PDH by downregulating pyruvate dehydrogenase kinase-2, which in turn results in PDH activation on the other hand (Refs Reference Boidot88, Reference Contractor and Harris89). In addition, p53 upregulates the expression of the E3 ubiquitin ligase Parkin, which ubiquitylates PKM2 and decreases its activity and thereby the glycolytic flux (Ref. Reference Liu90). In line with p53 negatively regulating glycolysis, p53 also promotes oxidative phosphorylation in the mitochondria. Synthesis of cytochrome c oxidase 2 (SCO2) is one of the genes that is induced in a p53-dependent manner and SCO2 protein is one of the cytochrome c oxidase assembly factors and thereby necessary for the proper function of the mitochondrial respiratory chain (Ref. Reference Matoba91). Apoptosis inducing factor (AIF) is another gene upregulated by p53 and the translated mitochondrial flavoprotein AIF is required for proper assembly of mitochondrial respiratory complex I (Ref. Reference Stambolsky92).
This shows that a growing body of evidence supports the role of p53 in regulating cellular metabolism and in particular promotes the reversion of the Warburg effect (Fig. 5). However, p53 is mutated in about 50% of cancers in which it leads to compromised oxidative phosphorylation and support of glycolysis.
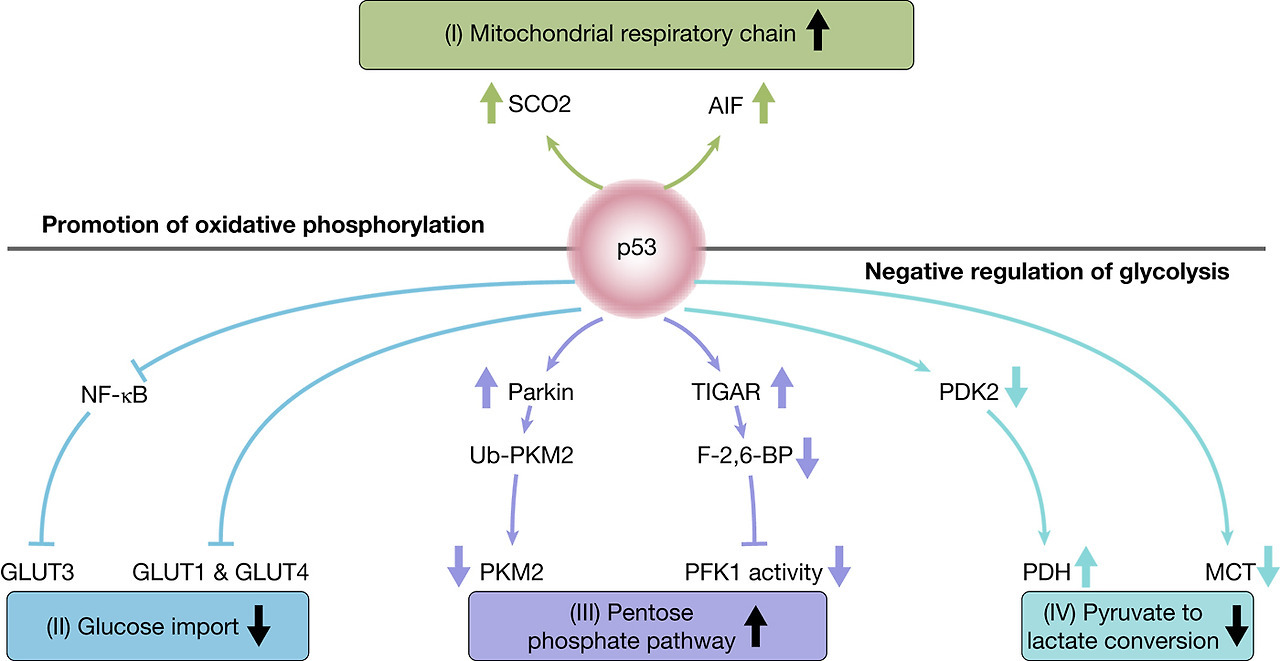
Fig. 5. Impact of p53 on glucose metabolism. Scheme of the pathways by which p53 promotes oxidative phosphorylation directly or through negative regulation of glycolysis. (I) P53 induces the expression of proteins implicated in the proper function of the mitochondrial respiratory chain: SCO2 and AIF. (II) P53 reduces glucose import through direct repression of GLUT1 and GLUT4 transcription and indirect repression of GLUT3 through inhibition of NF-κB. (III) P53 promotes glycolytic flux through the pentose phosphate pathway by downregulating PKM2 through the promotion of its ubiquitination and reducing PFK1 activity through F-2,6-BP depletion. (IV) P53 reduces the conversion of pyruvate to lactate by minimising lactate efflux through MCT downregulation and promoting the conversion of pyruvate to acetyl-CoA through the decrease of PDK2 activity and consequently increase in PDH activity.
Beyond Warburg: Krebs and glutamine metabolism
Cancer metabolism is a complex and flexible system involving the orchestration of energy metabolism, cell growth and proliferation with nutrients besides glucose, such as glutamine, also playing important roles in tumours. Glutamine is the most abundant amino acid accounting for more than 20% and 40% of the free amino acid pool in the plasma and muscle, respectively (Ref. Reference Bergstrom93).
Hans Krebs, who is probably more well-known for his characterisation of the tricarboxylic acid cycle (or Krebs' cycle), played a major role in elucidating glutamine metabolism (Ref. Reference Krebs94). In 1935, he published his findings on glutamine synthesis as an endothermic reaction that is catalysed by an enzyme, glutaminase, which exists in two distinct forms (Ref. Reference Krebs94). Glutamine is a conditionally essential amino acid, becoming essential under conditions that exceed the body's synthetic capabilities, especially in hyper-catabolic stress states, such as injury, sepsis and inflammation resulting in increased glutamine consumption by the gastrointestinal tract, immune cells, inflammatory tissue and kidney (Ref. Reference Lacey and Wilmore95). Glutamine is not only a precursor for a variety of biomolecules, such as proteins, nucleotides and amino sugars, but also plays a role in the acid–base balance because of being a precursor of urinary ammonia, functions as a nitrogen carrier between tissues, is involved in the regulation of glycogen synthesis in the liver and can work as respiratory fuel (Ref. Reference Krebs, Mora and Palacios96) (reviewed in Ref. Reference DeBerardinis and Cheng97). Several cancer cells have been shown to be addicted to glutamine, making it a prerequisite for culture conditions (Ref. Reference Eagle98) and this glutamine-dependency finding was also extended to the growth of certain tumours in vivo (exemplified in Refs Reference Abu Aboud99, Reference Son100, Reference Lampa101).
Glutamine metabolism in cancer
Glutamine is actively transported across the cell membrane by one of 14 membrane transporters belonging to four distinct gene families of the solute carrier (SLC) group transporters: SLC1, SLC6, SLC7 and SLC38 (Ref. Reference Bhutia and Ganapathy102). Among those, SLC1A5 has been heavily studied and shown to be upregulated in many solid cancer types, exemplified by but not limited to triple-negative breast cancer (Ref. Reference van Geldermalsen103), melanoma (Ref. Reference Wang104), neuroblastoma (Ref. Reference Ren105) or colorectal cancer (Ref. Reference Huang106). Another route of amino acid uptake in general is micropinocytosis. This internalisation process through vesicles has been shown to provide a route to contribute to glutamine-dependence by micropinocytic uptake of proteins in Ras-transformed pancreatic and urinary bladder cancers (Ref. Reference Commisso107).
After entering the cell, glutamine is metabolised to glutamate and an ammonium ion by glutaminase, an enzyme that exists in several tissue-specific isoforms and is encoded in humans by the genes GLS and GLS2 (Ref. Reference Mates, Campos-Sandoval and Marquez108). Through alternative splicing, GLS transcribes for two transcripts, translated into the mitochondrial kidney-type glutaminase (KGA) and glutaminase C (GAC), while GLS2 encodes the two proteins GAB and liver-type glutaminase through a surrogate promoter mechanism (Refs Reference Mates, Campos-Sandoval and Marquez108, Reference Martin-Rufian109). GAC is upregulated in several solid cancers, such as breast (Ref. Reference Cassago110), lung (Ref. Reference van den Heuvel111), colon (Ref. Reference Huang112) and prostate (Ref. Reference Pan113).
Following the conversion from glutamine to glutamate by glutaminases, glutamate is further metabolised to α-KG by either glutamate dehydrogenase (GLUD) or aminotransferases. Although GLUD catalyse the reversible deamination of glutamate by releasing ammonia, aminotransferases, according to their name, transfer the nitrogen onto other biomolecules, such as pyruvate or 3-phosphohydroxypyruvate, as within the second step of de novo serine synthesis (Ref. Reference Moreadith and Lehninger114). In tumours, glutamate is mainly metabolised by aminotransferases, whose expression is upregulated while GLUD expression is low (Ref. Reference Coloff115). Generated α-KG can be further metabolised to the oncometabolite 2-HG, a reaction catalysed by IDH as described earlier.
Similar to the Warburg effect, there are several oncogenes, such as KRAS, Myc and p53, that contribute to reprogramming glutamine metabolism in cancer and a few examples will be given herein. KRAS enhances the diversion of glutamine into the TCA cycle or transamination in order to sustain the synthesis of biomolecules (Ref. Reference Gaglio116). In pancreatic ductal adenocarcinoma (PDAC), oncogenic KRAS has been shown to promote aspartate transaminase (GOT1) expression, while reducing GLUD1 expression, thereby supporting the irreversible deamination of glutamate (Ref. Reference Son100). On similar lines, induced Myc expression in mouse embryonic fibroblasts leads to rewiring of their metabolism and an addiction to glutamine and stimulation of the mitochondrial glutamine catabolism (Ref. Reference Wise117). Further studies on Myc-regulated glutamine metabolism reveal that Myc transcriptionally represses miR-23a and miR-23b, which leads to increased expression of mitochondrial glutaminases in lymphoma and prostate cancer cell lines (Ref. Reference Gao118). Recently Myc has also been reported to support glutamine synthesis through increasing glutamine synthase expression initiated by promoter demethylation, which then leads to an increased usage of glutamine in nucleotide and protein synthesis (Ref. Reference Bott119). P53 has been shown to induce the expression of glutaminase 2 isoforms, which results in shifting glucose metabolism towards oxidative phosphorylation and reduction of tumour cell growth (Ref. Reference Hu120).
Collaboration of glucose and glutamine metabolism in cancer
With the shift of cancer cell metabolism towards the Warburg effect, that is, reduced glycolytic flux through the mitochondria and lower ATP production, glutamine is able to step in as an alternative carbon source in order to guarantee sufficient energy production and synthesis of biomolecules (nucleic acids and proteins) necessary for proliferation (Fig. 6).
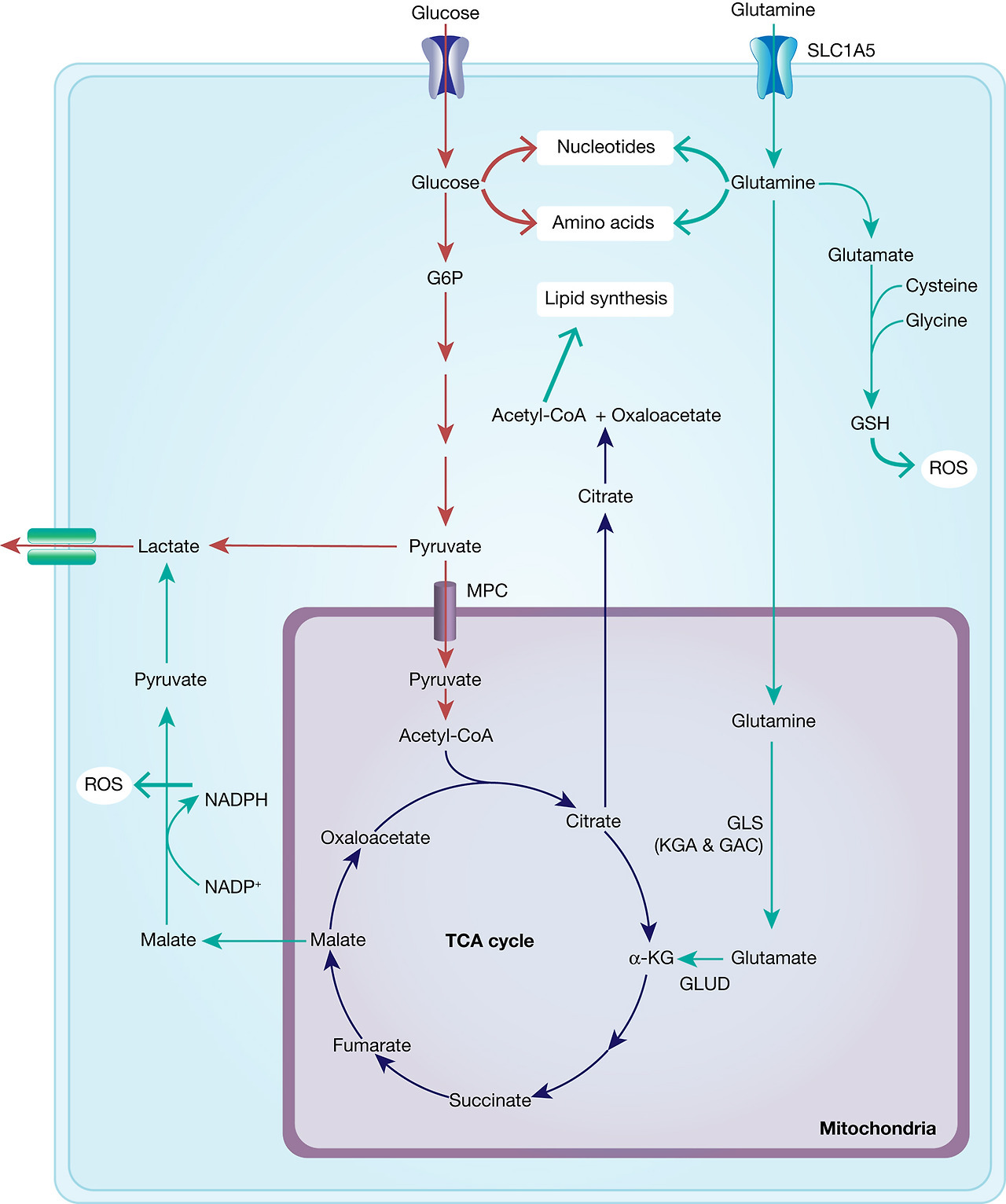
Fig. 6. Interplay between glucose and glutamine metabolism to drive cancer growth. Glucose is transported into the cells and mainly metabolised into pyruvate and lactate and thereby contributes to nucleotide and amino acid synthesis. Glutamine is equally transported into the cells and metabolised to glutamate and α-KG, fuelling into the TCA cycle and thus into ATP generation and lipid synthesis. TCA-cycle-derived malate is further metabolised to pyruvate, thereby generating NADPH and thus contributing to maintaining redox balance. In addition, glutamate fuels into GSH synthesis, which is an important ROS scavenger.
Metabolic studies with 13C-labelled glutamine and glucose in the human GBM cell line SF188 have shown that a large part of glutamine is replenishing the TCA cycle with glutamine-derived α-KG (anaplerosis) (Ref. Reference DeBerardinis121). In line with this, inhibition of pyruvate transport into the mitochondria via the mitochondrial pyruvate carrier in glioma cells activates GLUD, which catalyses the reaction of glutamate to α-KG in the mitochondria, fuelling into the TCA cycle (Ref. Reference Yang122). In addition, glutamine-derived carbon can also support lipid synthesis as the TCA cycle intermediate, citrate, is exported into the cytosol where it is cleaved into acetyl-CoA and oxaloacetate, a necessary precursor for lipid synthesis. While this pathway has been reported to be predominant in cancer cells under hypoxia (Ref. Reference Metallo123), glucose-derived citrate is considered to be the main source for acetyl-CoA under normoxic conditions (Ref. Reference Hatzivassiliou124).
Glutamine has also an important role in the regulation of oxidative stress. Malate, a biomolecule generated within the TCA cycle, can be exported from the mitochondria and converted to pyruvate by malic enzyme, a process that generates NADPH and thus contributes to the cellular redox balance. In human PDAC cells, glutamine-derived aspartate is converted to oxaloacetate, which is subsequently converted into malate then pyruvate and with the last catalytic step generating NADPH (Ref. Reference Son100). Furthermore, glutamate is used in the de novo synthesis of reduced glutathione (GSH), an essential scavenger of reactive oxygen species (ROS) and depletion of glutamine has been shown to reduce the cellular GSH concentration in Myc-driven cells (Ref. Reference Yuneva125). In anchorage-independent growth conditions, IDH1-dpendent reductive carboxylation of glutamine was shown to generate NADPH in the mitochondria and thereby suppress mitochondrial ROS (Ref. Reference Jiang126).
Despite the interplay of glutamine and glucose metabolism, the different pathways are not necessarily co-regulated. Although the PI3K/AKT signalling pathway stimulates glucose uptake and metabolism, glutamine uptake and metabolism is independent of this signalling cascade in Myc-dependent glioma cells (Ref. Reference Wise117).
Therapeutic strategies arising from the Warburg effect and altered glutamine metabolism
The altered metabolic pathways, reflecting the demands of highly proliferating cancer cells and their tumour environment, may be exploited diagnostically and therapeutically. It should be noted that there are more metabolic pathways, besides glucose and glutamine addiction, that are altered in cancer, which represent additional directions for the development of cancer therapeutics by targeting cancer metabolism, but are beyond the scope of this review.
Imaging: diagnosis and monitoring of tumours
The first medical procedure really based on Warburg's findings is 18F-deoxyglucose positron emission tomography (18FDG-PET), which makes use of increased glucose and also 18FDG uptake in most cancers compared with normal tissue and was implemented in the clinic in the 1980s (Ref. Reference Conti127).
With the emerging evidence for the role of glutamine and increased glutamine uptake in tumours, several studies have investigated glutamine-based tracers for PET scans. 5-11C-(2S)-glutamine and 18F-(2S,4R)-4-fluoroglutamine (18FG) have been proposed as complementary tools to guide glutamine-targeted therapies with 18FG showing a different tumour-to-background contrast compared with 18FDG in glioma patients (Ref. Reference Zhu128). 18F-Gln-BF3 is another tracer that has shown significant uptake in xenograft studies (Ref. Reference Li129) (Table 1, Fig. 7).
Table 1. Labelled glucose and glutamine derivatives used for imaging for cancer diagnosis and progression
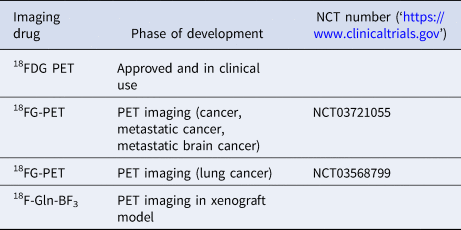
FDG, fluorodeoxyglucose; FG, fluoroglutamine; Gln, glutamine; PET, positron emission tomography.
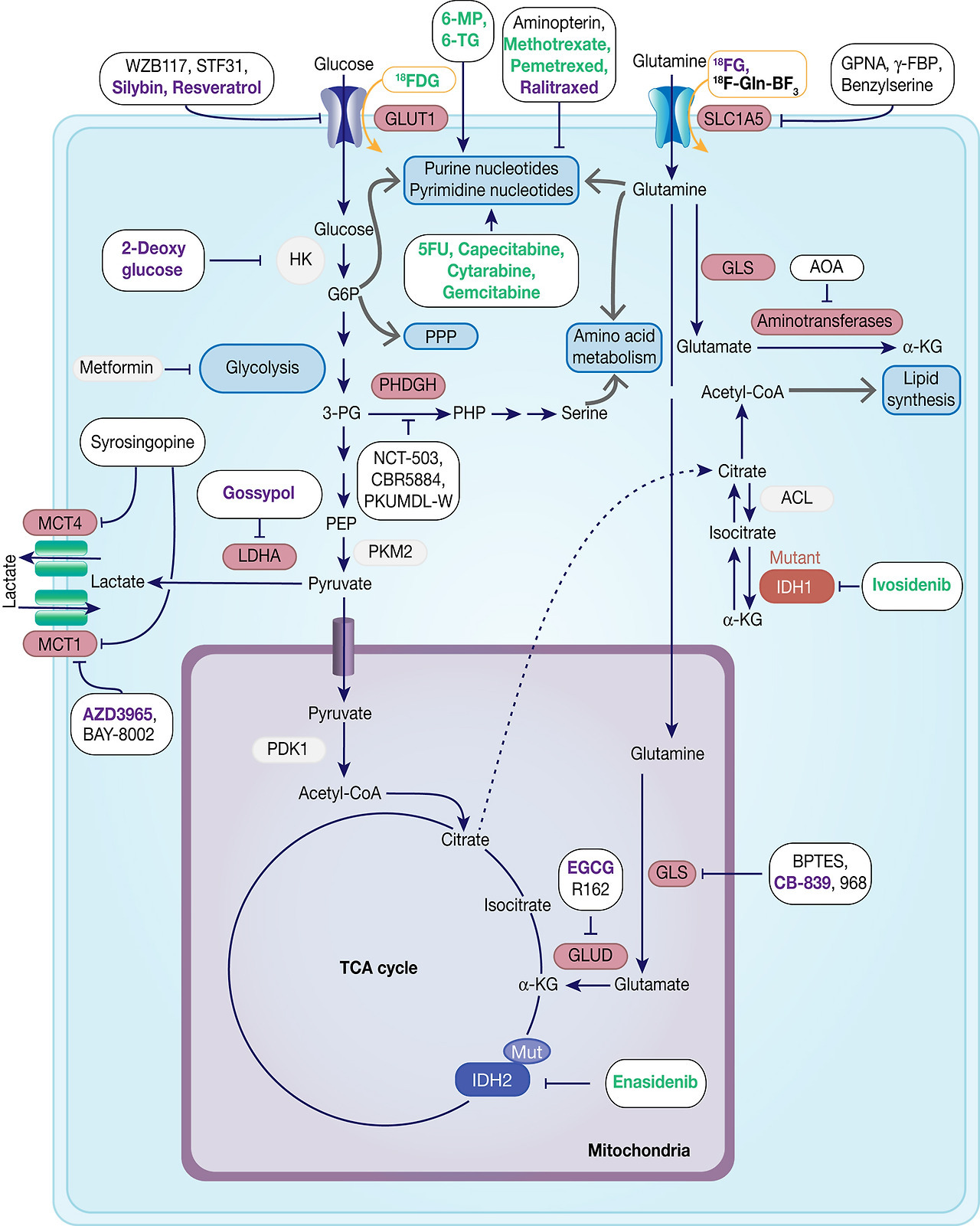
Fig. 7. Therapeutic targets in cancer metabolism. Metabolic enzymes which are under preclinical investigation are highlighted in red. Inhibitors are framed in black, whereas compounds used for imaging are framed in orange. Compounds which are under development are in black, compounds in clinical studies are in purple and FDA-approved drugs are in green.
Antimetabolites
Chemotherapeutic agents targeting metabolic enzymes have an even longer history in the treatment of neoplastic disease. In the late 1940s, successful targeting of cancer cell metabolism was already achieved using the antifolate drug aminopterin to induce remission in children with acute lymphoblastic leukaemia (ALL) (Ref. Reference Farber130). More antifolate drugs, such as methotrexate, were developed and were shown to exhibit their antitumour effect through inhibition of dihydrofolate reductase, which subsequently leads to the loss of reduced folates and in turn inhibits thymidylate and purine synthesis causing cytostasis or cell death (Ref. Reference Purcell and Ettinger131). Antifolate drugs have a broad application in the treatment of different solid tumours and haematologic malignancies and there has been a continuous effort in the development of the next generation of antifolates, such as raltitrexed and pemetrexed (Ref. Reference Gonen and Assaraf132).
Analogues of purines (6-mercaptopurine, azathioprine, 6-thioguanine) and pyrimidine (5-fluorouracil, cytarabine, gemcitabine) are also used extensively in cancer therapy, often in combination with DNA repair chemotherapeutics. They exert their antiproliferative activity by blocking nucleotide metabolism and becoming misincorporated into DNA following intracellular conversion to their corresponding nucleotides (Refs Reference Karran and Attard133, Reference Longley, Harkin and Johnston134, Reference Parker135) (Table 2, Fig. 7).
Table 2. List of approved drugs or preclinical tools among anti-folates and nucleotide analogues
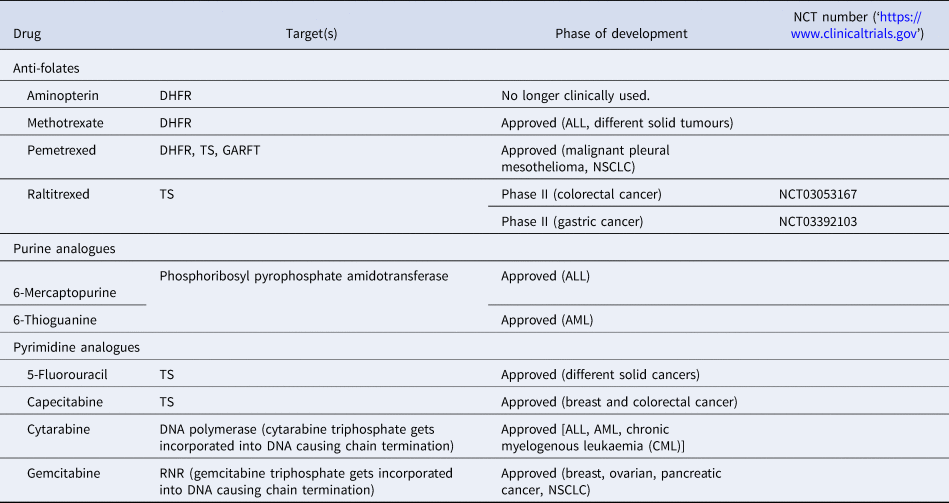
ALL, acute lymphoblastic leukaemia; AML, acute myeloid leukaemia; DHFR, dihydrofolate reductase; GARFT, glycinamide ribonucleotide formyltransferase; NSCLC, non-small cell lung cancer; RNR, ribonucleotide reductase, TS, thymidylate synthase.
Glucose metabolism
Based on an increasing understanding and interest in the Warburg effect and the importance of glucose metabolism in cancer cells, the pharmacological intervention of these pathways has come into more focus (Table 3, Fig. 7). Many cancers show upregulation of different glucose transporters, such as GLUT1, 3 and 4 and this fact is exploited in 18FDG-PET imaging. Several GLUT1 inhibitors from different chemical classes have been developed, such as WZB117, STF31, Silybin and Resveratrol showing promising results in in vitro experiments in different cancer cell lines (Ref. Reference Labak136) with Silybin also having been investigated in phase I clinical studies in prostate cancer (Ref. Reference Flaig137). 2-Deoxyglucose, in contrast, was established as a molecule that is able to enter cells via the glucose transporters but cannot be metabolised beyond 2-deoxyglucose-6-phosphate (2-DG-P) and therefore accumulates (Ref. Reference Woodward and Hudson138). 2-DG-P competitively inhibits phosphoglucose isomerase as well as hexokinase in a non-competitive manner and thereby slows further glucose uptake and metabolism leading to cancer cell death in vitro (Refs Reference Wick139, Reference Crane and Sols140). Although several preclinical studies demonstrated anti-proliferative effects in different cancers, these results could not be translated into clinical settings for 2-DG monotherapy (Ref. Reference Voss141). One major limitation for the usage of 2-DG is its toxicity associated with hypoglycaemia. This toxicity is potentially due to more than one mechanism as 2-DG has been shown to interfere with several biological processes beyond glycolysis, such as induction of oxidative stress, interference with N-linked glycosylation in the endoplasmic reticulum or induction of autophagy (Refs Reference Voss141, Reference Zhang142).
Table 3. List of preclinical tools and compounds in clinical trials for targets within glucose metabolism
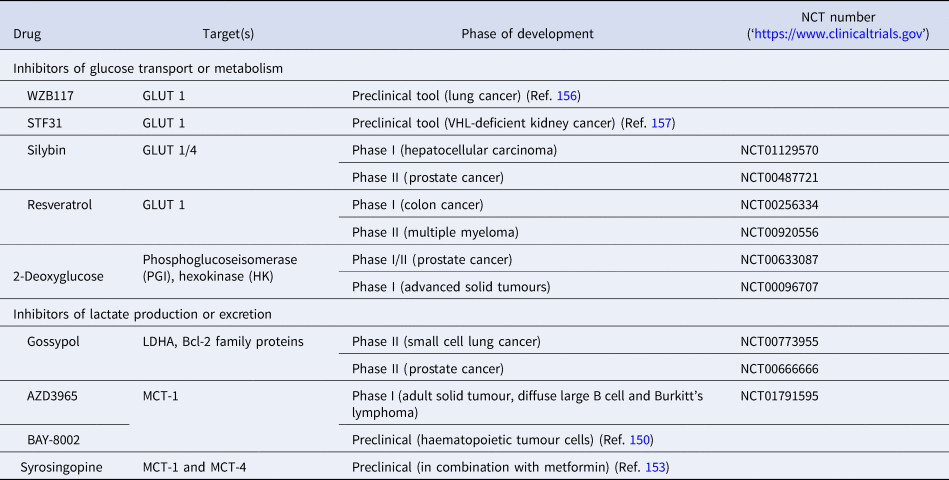
GLUT, glucose transporter 1; LDHA, lactate dehydrogenase; MCT, monocarboxylate transporter.
Another route currently explored to target aerobic glycolysis in caner is through interference with lactate production or excretion. LDHA catalyses the conversion of pyruvate to lactate and as outlined before, LDHA expression is upregulated by HIF-1 and c-Myc. Many cancers were found to have higher levels of LDHA compared with normal tissue (Ref. Reference Goldman, Kaplan and Hall143) and LDHA has been shown to be required for initiation, maintenance and progression of various tumours making it an interesting cancer target (Refs Reference Xie144, Reference Fantin, St-Pierre and Leder145). To date, several inhibitors of LDHA have been reported and mainly validated in biochemical or cell-based models as pharmacokinetic properties or selectivity were not good enough for in vivo studies (Ref. Reference Rani and Kumar146). Among the known LDHA inhibitors is the natural product gossypol, which was investigated in phase I/II clinical studies for different cancers, but is also a reported pan-inhibitor of anti-apoptotic Bcl-2 family protein members (‘https :// www.clinicaltrials.gov’, Refs Reference Rani and Kumar146, Reference Wang147). Following lactate formation, MCT, especially 1 and 4, are responsible for transporting lactate out of the cells, thereby being part of metabolic reprogramming in cancer and thus attractive targets for antitumour therapy (Refs Reference Sonveaux73, Reference Izumi148). Hence, MCT1 inhibition has been shown to lead to the accumulation of intracellular lactate resulting in a decrease in intracellular pH and disabling glycolysis and tumour cell growth (Ref. Reference Doherty72). In a few tumours, lactate import was also observed to be important for tumour growth under glucose-deprived conditions in which lactate fuels into the oxidative phosphorylation pathway (Ref. Reference Sonveaux149). The only promising small-molecule MCT inhibitors to date are BAY-8002 and AZD3965 (Refs Reference Quanz150, Reference Curtis151). Both are MCT1-specific inhibitors with AZD3965 showing potent antitumour activity in a Burkitt's lymphoma xenograft model, whereas treatment with BAY-8002 only resulted in tumour stasis (Refs Reference Quanz150, Reference Curtis151). AZD3965 is currently undergoing phase I clinical trials in patients with advanced solid tumours, B cell lymphoma or Burkitt's lymphoma (Table 3). A challenge in the development of MCT inhibitors for the treatment of cancer is the potential of drug resistance because of overlapping functions within the MCT family, such as functional redundancy of MCT1 and 4. In this context, it has been shown that MCT4 overexpression leads to AZD3965 resistance, whereas MCT4 knockdown resulted in AZD3965 sensitisation (Ref. Reference Polanski152). Recently, syrosingopine has been reported to be a dual inhibitor of MCT1 and MCT4 and to be synthetically lethal in combination with metformin in cancer cells (Refs Reference Benjamin153, Reference Benjamin154). Initially developed and widely used for the treatment of Type II diabetes, metformin has been shown to have multiple targets in glycolysis and is now repurposed and being investigated for the treatment of different cancers, such as in a currently recruiting phase II clinical trial for prostate cancer (NCT03137186) (Ref. Reference Kourelis and Siegel155).
Oncoenzymes: IDH and PHGDH
The ‘oncoenzymes’ presented here: IDH and PHGDH also present interesting targets for cancer therapy that are currently been exploited. Ivosidenib (Tibsovo®) and enasidenib (Idhifa®) are orally available, selective, small-molecule inhibitors of mutated cytosolic IDH1 or IDH2, respectively, which, in line with the presented biology on IDH, prevent the formation of the oncometabolite 2-HG (Refs Reference Popovici-Muller158, Reference Shih159). Evosidenib and ivosidenib have both recently received US Food and Drug Administration (FDA)-approval for treatment of patients with relapsed or refractory AML and are still under further clinical investigation for solid tumours, cholangiocarcinoma and haematological malignancies (Refs Reference Dhillon160, Reference Dugan and Pollyea161). To date several other targeted inhibitors of mutant IDH1 and/or IDH2 are under development and some are currently investigated in clinical phases I-III (Table 4) (Refs Reference Raineri and Mellor162, Reference Buege, DiPippo and DiNardo163).
Table 4. List of preclinical tools and compounds in clinical trials for IDH and PHGDH
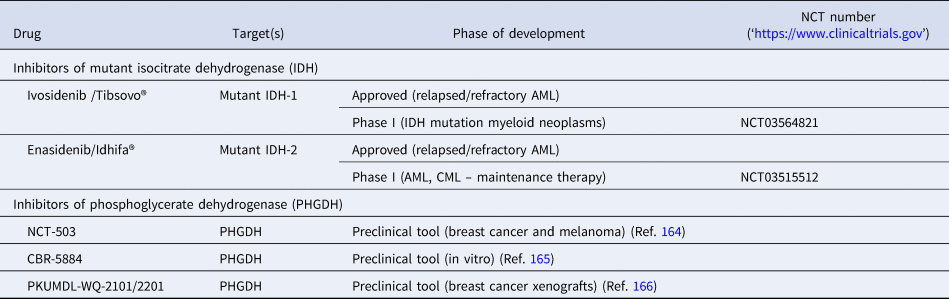
AML, acute myeloid leukaemia; CML, chronic myeloid leukaemia; IDH, isocitrate dehydrogenase; PHGDH, 3-phosphoglycerate dehydrogenase.
With PHGDH's proposed role in tumourigenesis and tumour progression in several solid cancers, the focus has been on the development of small-molecule inhibitors targeting PHGDH. Fragment-based approaches have been reported to target the substrate and cofactor-binding pockets of PHGDH, yielding novel starting points for the development of PHGDH inhibitors (Ref. Reference Unterlass167) as well as a more elaborate inhibitor from AstraZeneca with a reported Kd (SPR) of 0.18 µm (Ref. Reference Fuller168). In addition, two non-competitive inhibitors, CBR-5884 (Ref. Reference Mullarky165) and NCT-503 (Ref. Reference Pacold164) have been proposed with IC50 values of 33 and 2.5 µm, respectively. Of these inhibitors, only NCT-503 was investigated in vivo because of poor plasma stability of CBR-5884. In the in vivo study with NCT-503 in mice bearing MDA-MB-468 (PHGDH-high expressing breast cancer cells) orthotopic xenografts, the tumour burden was reduced by 50% following daily treatment (40 mg/kg, IP) (Refs Reference Pacold164, Reference Mullarky165). In addition, a series of pyrazole-5 carboxamide with IC50 < 50 µM derivatives have been disclosed in a patent (WO2016/040449A1) as well as PHGDH inhibitors, PKUMDL-WQ-2101/2201, that bind to allosteric sites of PHGDH and could significantly inhibit tumour growth in breast cancer xenografts (Ref. Reference Wang166).
Glutamine metabolism
With glutamine being an important nutrient for cancer cells, but at the same time a non-essential amino acid under normal growth conditions, preventing glutamine import into cells provides a valid cancer targeting strategy (Table 5, Fig. 7). Among the transporters for glutamine, SLC1A5 has been predominantly studied in cancer and shown to be frequently upregulated. The glutamine analogue L-γ-glutamyl-p-nitroanilide (GPNA) was among the first SLC1A5 inhibitors to be proposed (Ref. Reference Esslinger, Cybulski and Rhoderick169) and has been shown to reduce glutamine uptake in several cancer types, such as NSCLC (Ref. Reference Hassanein170), myeloma cells (Ref. Reference Bolzoni171) or prostate cancer (Ref. Reference Wang172). However, recent studies suggest that GPNA is a non-selective SLC1A5 inhibitor that also affects other sodium-dependent carriers of the SNAT family (Ref. Reference Broer, Rahimi and Broer173) as well as the sodium-independent neutral amino acid transporter LAT1 (Ref. Reference Chiu174).
Table 5. List of preclinical tools and compounds in clinical trials for targets within glutaminolysis

AOA, aminooxyacetate; BPTES, bi-2-(5-phenylacetamido-12,4-thiadiazol-2-yl)ethyl sulphide; EGCG, pigallocatechin gallate; γ-FBP, γ-folate-binding protein; GPNA, L-γ-glutamyl-p-nitroanilide.
Other reported SLC1A5 inhibitors are benzylserine and benzylcysteine, which have been shown to are weak (mM-affinity for SLC1A5), competitive inhibitors of SLC1A5 (Ref. Reference Grewer and Grabsch175), but are also non-selective and in the case of benzylserine also affect other amino acid transporters, such as LAT1 (Ref. Reference Wang104). Despite weak inhibitory affinity, benzylserine has been shown to decrease breast cancer cell viability and cell progression (Ref. Reference van Geldermalsen176).
The proline derivative γ-folate-binding protein is a newly described SLC1A5 inhibitor, obtained from a virtual screening campaign and shown to decrease melanoma cancer cell viability using compound doses in the low-mM range (Ref. Reference Colas177).
Glutaminase 1 (GLS1) isoforms, especially GAC, have been found to be upregulated in different cancers and suppression by genetic knockdown showed antitumour activity, thus validating glutaminases as promising targets for cancer therapy. In this context, bi-2-(5-phenylacetamido-12,4-thiadiazol-2-yl)ethyl sulphide (BPTES) has been reported and identified as an allosteric KGA and GAC inhibitor that blocks the respective tetramer in an inactive conformation, but does not affect the GLS2 isoforms (Refs Reference Newcomb178, Reference DeLaBarre179, Reference Robinson180). Although several studies report antitumour activity of BPTES in different tumour types, its usage in clinical studies is limited by moderate potency, metabolic instability and low solubility (Ref. Reference Gross181). In order to improve these properties, BPTES derivatives were investigated and led to CB-839, a potent, selective and orally bioavailable inhibitor of the two main splice variants of GLS1: KGA and GAC, that is currently investigated in phase I and II clinical trials (Table 5) (Refs Reference Gross181, Reference Liang, Bromley and Orford182). In search of glutaminase inhibitors with a different modus operandi, compound 968 was reported to bind to the inactive, monomeric GAC and preventing it from undergoing conformational changes to an activated state (Refs Reference Wang183, Reference Stalnecker184).
The metabolism of glutamate to α-KG is performed by GLUD or aminotransferases and as α-KG is not only a precursor for the oncometabolite 2-HG, but also fuels into the TCA cycle, its production is another attractive target for cancer therapy.
The green tea polyphenol, epigallocatechin gallate (EGCG) was reported to inhibit GLUD in the nM-range and to inhibit the growth of N-Myc amplified neuroblastoma cells and c-Myc overexpressing glioma cells (Refs Reference Li185, Reference Qing186, Reference Yang187). However, as EGCG inhibits a variety of NADPH-requiring enzymes, a screening for more selective GLUD inhibitors revealed the purpurin analogue R162 (Ref. Reference Jin188). R162 was subsequently shown to significantly reduce cell viability in human lung, breast and leukaemia cell lines (Ref. Reference Jin188). Aminooxyacetate (AOA) is a non-specific transaminase inhibitor that initially has been investigated as palliative treatment in tinnitus (Refs Reference Reed189, Reference Guth190) and had failed in a small trial with seven patients in Huntington's disease (Ref. Reference Perry191). In preclinical studies for cancer therapy, AOA has been used to inhibit the anaplerotic use of glutamine in the TCA cycle and has shown to decrease tumour growth in breast cancer xenograft studies (Refs Reference Thornburg192, Reference Korangath193).
Concluding remarks and future directions
The discovery of aerobic glycolysis by Warburg was certainly a milestone discovery in the area of cancer metabolism, but also just one aspect of a complex metabolic network. There is an increasing body of literature and evidence showing that cancer is a metabolic disease and that metabolic dependencies in cancer offer an exciting new area of research with great potential for the development of novel therapeutics, such as the renewed focus on glutamine metabolism shows. As a tumour represents a heterogeneous mixture of cells and accumulates further mutations during division and expansion, it will be difficult to erase a tumour completely by targeting individual mutated gene products. In this regard, targeting metabolic dependencies of cancers, such as the Warburg effect or glutamine dependence, could provide promising new avenues for developing new cancer treatments.
However, the metabolic network is also very intricate and complex so that a clear understanding of the metabolic alterations in tumours within their context is necessary. As metabolic pathways are evolutionarily conserved, it is important to consider potential toxicities when developing metabolic inhibitors. Nevertheless, for other diseases, metabolic inhibitors, such as metformin for Type II diabetes, have successfully been developed with sufficient safety profiles, indicating that targeting cancer metabolism with limited toxicities should be achievable.
Next to the development of novel inhibitors, it is necessary to establish non-invasive methods for patient stratification as not all tumours rely on the same metabolic pathways. Progression biomarkers and early detection of resistance mechanism will be a key factor as cancer metabolism has been shown to be an adaptive and dynamic system influenced by the tumour micro-environment.
One has to remember that several anticancer chemotherapeutic agents used to date are drugs targeting tumour metabolism, such as the antifolates or nucleotide analogues. Together with a strong research effort that has led to several clinical trials for inhibitors targeting metabolic pathways to date, there is substantial potential in pursuing these new avenues for effective new cancer treatments.