문치연에서 비문증은 어렵지 않게 호전중!!
한의사(이름, 한의원명)만 들어올 수 있어요.
https://open.kakao.com/o/g6qEAsUg
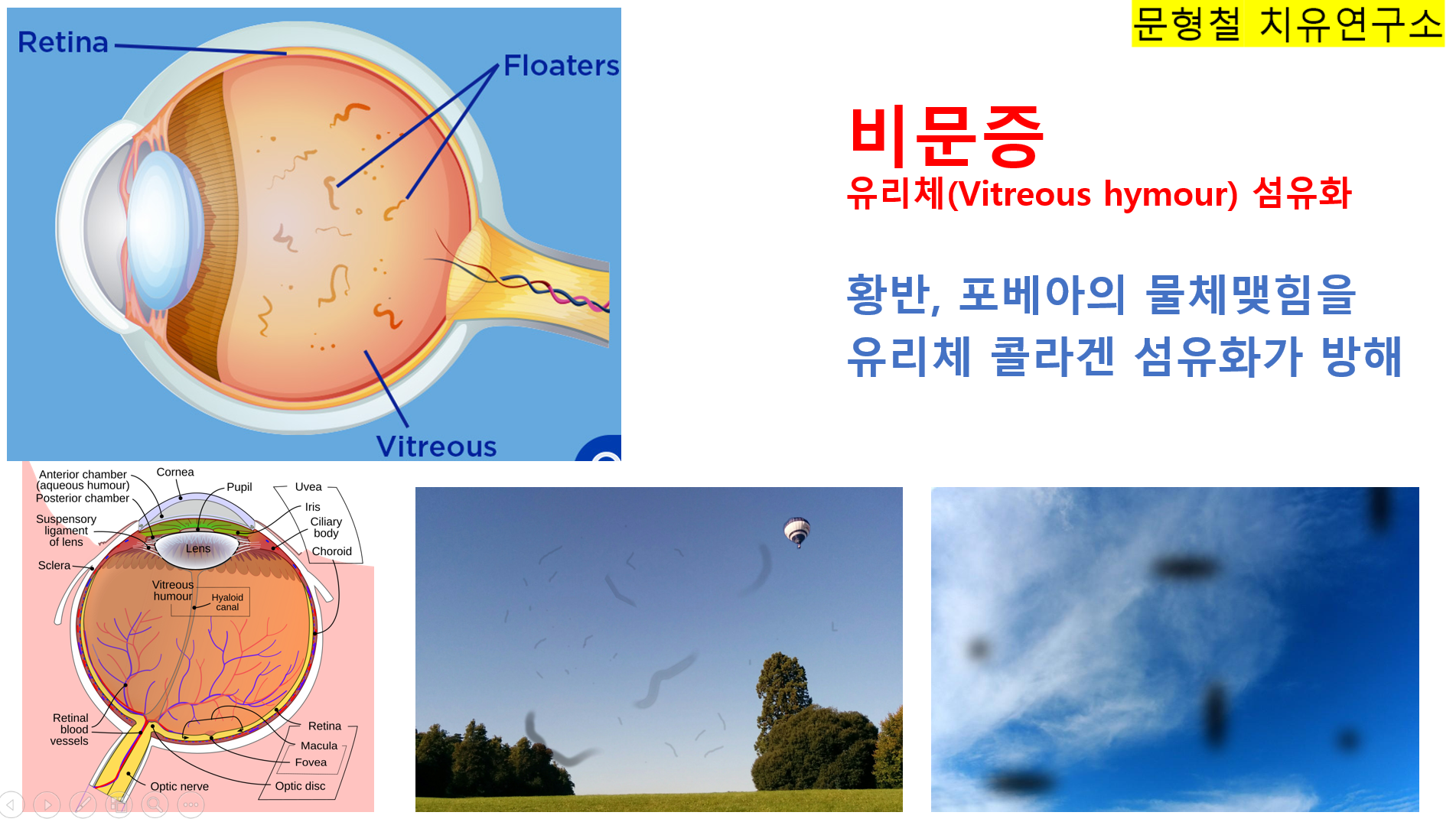

유리체(또는 vitreous body)는 눈의 수정체와 망막 사이의 넓은 공간을 채우고 눈의 형태를 유지하며 영양을 공급하는 투명한 젤 같은 물질로, 주로 물, 콜라겐, 히알루론산으로 구성되어 있습니다.
나이가 들면서 유리체는 액화되고 수축할 수 있으며, 이로 인해 부유물(점, 선)이나 섬광 현상이 발생할 수 있습니다. 이는 후부 유리체 박리(PVD)나 망막 문제로 이어질 수 있으며, 심각한 문제의 경우 유리체 절제술과 같은 치료가 필요할 수 있습니다.
구성 및 기능
구성: 약 99%가 물이며, 구조 단백질(콜라겐)과 히알루론산이 젤 같은 농도를 만듭니다.
기능: 안구의 구형 모양을 유지하고, 망막을 지지하며, 빛 전달을 돕습니다.
구성:
약 99%가 물이며, 구조 단백질(콜라겐)과 히알루론산이 젤 같은 농도를 만듭니다.
기능:
안구의 구형 구조 유지, 망막 지지, 빛 전달 보조.
노화 관련 변화 (유리체 퇴행)
액화: 젤이 점차 액체로 변하며 덩어리와 빈 공간을 형성합니다.
유리체 혼탁: 응축된 섬유가 움직이는 점, 실, 그림자로 나타납니다.
섬광: 수축된 섬유가 망막을 당겨 섬광을 유발합니다.
후부 유리체 박리(PVD): 유리체가 망막에서 분리되며, 종종 갑작스러운 부유물과 섬광 증가로 나타남.
합병증 및 치료
합병증:
PVD는 망막열공, 출혈(유리체 출혈), 황반공을 유발할 수 있음.
유리체 절제술:
유리체를 수술적으로 제거하는 것으로, 주로 망막열공이나 박리를 치료하기 위해 시행되며, 제거된 공간에는 가스, 오일 또는 식염수를 주입합니다.
검사 방법
안과 의사는 동공 확장 검사를 실시합니다. 동공 확장 안약을 점안하여 유리체와 망막을 관찰함으로써 박리나 열공 여부를 확인합니다.
메이요 클리닉 설명
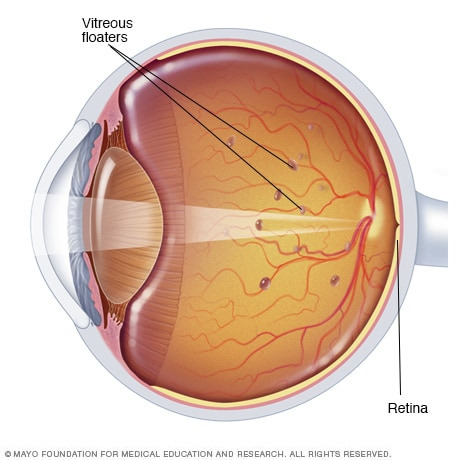
Eye floaters are spots in your vision. They may look to you like black or gray specks, strings, or cobwebs. They may drift about when you move your eyes. Floaters appear to dart away when you try to look at them directly.
Most eye floaters are caused by age-related changes that occur as the jelly-like substance (vitreous) inside your eyes liquifies and contracts. Scattered clumps of collagen fibers form within the vitreous and can cast tiny shadows on your retina. The shadows you see are called floaters.
If you notice a sudden increase in eye floaters, contact an eye specialist immediately — especially if you also see light flashes or lose your vision. These can be symptoms of an emergency that requires prompt attention.
눈 속의 부유물은
시야에 나타나는 점들입니다.
검은색이나 회색의 점, 실, 거미줄처럼 보일 수 있습니다.
눈을 움직일 때 함께 떠다니기도 합니다.
부유물은 직접 바라보려고 하면 재빨리 사라지는 것처럼 보입니다.
대부분의 눈 속 부유물은
눈 안의 젤리 같은 물질(유리체)이 액화되고 수축하면서 발생하는 노화 관련 변화로 인해 생깁니다.
유리체 내부에 흩어진 콜라겐 섬유 덩어리가 형성되어
망막에 미세한 그림자를 드리울 수 있습니다.
이 그림자가 바로 부유물입니다.
| 비문증(eye floaters)은 일반적으로 황반변성(macular degeneration)의 초기 증상이 아닙니다. 두 질환은 눈의 다른 부분에서 발생하며 원인도 다릅니다. 비문증은 대부분 노화로 인해 눈 속의 유리체(젤리 같은 물질)가 수축하면서 작은 부유물들이 생겨 망막에 그림자를 드리우는 현상입니다. 대개 무해하지만, 갑자기 새로운 비문증이 많이 생기거나 빛 번쩍임이 동반되면 망막 박리 같은 심각한 안과 질환의 신호일 수 있으므로 즉시 안과 검진을 받아야 합니다. 황반변성은 망막 중심부인 황반이 손상되는 질환으로, 주로 중심 시력 저하, 사물이 휘어져 보이거나(선이 물결 모양으로 보임), 시야 중심에 공백이 생기는 등의 증상을 유발합니다. 초기 단계에는 특별한 증상이 없을 수도 있습니다. |
증상
눈의 부유물 증상은 다음과 같습니다:
- 시야에 어두운 점이나 투명한 실 모양의 부유물로 나타나는 작은 형태
- 눈을 움직일 때 함께 움직이는 점으로, 이를 보려고 하면 시야에서 빠르게 사라짐
- 푸른 하늘이나 하얀 벽과 같은 밝은 배경에서 가장 두드러지게 보이는 점
- 결국 가라앉아 시야 밖으로 떠내려가는 작은 모양이나 실
비문증(유리체 부유물, vitreous floaters)은
눈 속 유리체의 콜라겐 섬유가 응집되어 시야에 그림자나 점처럼 보이는 증상으로,
주로 후유리체박리(PVD)와 관련이 있습니다.
아래에서 유병률, 병기, 예후에 대해 설명하겠습니다.
주요 출처는 2023~2026년 사이의 연구들로, PubMed와 관련 저널에서 추출했습니다.
유병률 (Prevalence)
비문증은 흔한 증상으로,
일반 인구에서 자가 보고된 유병률은 76%에서 87%에 달합니다.
이는 나이 증가, 근시, 외상, 염증 등과 관련이 있으며,
특히 스마트폰 사용자 설문조사에서 76%가 비문증을 경험했다고 보고되었고,
이 중 33%가 시각 장애를 유발한다고 느꼈습니다.
후유리체박리의 유병률은 50-59세에서 24%,
80-89세에서 87%로 나이와 함께 급증합니다.
젊은 층(특히 근시 환자)에서 증가 추세를 보이며,
전체 인구의 2/3가 영향을 받을 수 있습니다.
병기 (Staging/Classification)
비문증의 주요 원인인 후유리체박리의 병기는 Kakehashi 등의 분류 체계에 따라 5단계로 나뉩니다. 이는 슬릿램프 현미경 검사와 OCT(광간섭 단층촬영)를 기반으로 하며, 유리체의 박리 정도를 평가합니다:
- Stage 0: 후유리체박리 없음 (No PVD).
- Stage 1: 주변부(황반 외)에서 불완전한 박리, 최대 3사분면 (Incomplete perifoveal PVD in up to 3 quadrants).
- Stage 2: 모든 사분면에서 주변부 박리, 하지만 황반과 시신경 유두에 여전히 부착 (Incomplete perifoveal PVD in all quadrants, attached to fovea and optic disc).
- Stage 3: 후극부(황반 주변)에서 불완전한 박리, 시신경 유두에 부착 (Incomplete PVD over posterior pole, attached to optic disc).
- Stage 4: 완전한 후유리체박리, Weiss ring(유리체 고리) 관찰 가능 (Complete PVD).
이 분류는 나이와 근시에 따라 진행되며, 젊은 근시 환자에서 초기 단계(Stage 1-2)가 더 흔합니다. 비문증 증상은 Stage 1부터 나타날 수 있지만, 초기 단계는 무증상일 수 있습니다.
예후 (Prognosis)
비문증의 예후는 대부분 양성(benign)으로,
합병증 없는 경우 시각 위협이 되지 않습니다.
증상(부유물, 섬광)은 보통 3개월 이내에 호전되거나 적응되며,
6개월 이상 지속될 수 있지만
자연적으로 사라지거나 덜 신경 쓰이게 됩니다.
그러나
일부 환자(특히 젊은 층)에서는 삶의 질 저하를 유발하며,
불안, 우울, 독서/운전 장애 등을 일으킬 수 있습니다.
연구에 따르면,
환자들은 증상 제거를 위해 사망 위험 11%나 실명 위험 7%를 감수할 의향이 있을 정도로 부담을 느낍니다.
합병증(망막 열상, 출혈 등)이 발생하면 예후가 나빠질 수 있으며,
치료(유리체절제술 등) 후 백내장 진행(75-100% 환자)이 흔합니다.
젊은 근시 환자에서 만성적일 수 있으나,
적절한 관리(관찰, 영양 보충, 수분 섭취)로 개선 가능합니다.
최신 논문 추천
최근(2023-2026) 연구 중 비문증의 유병률, 병기, 예후를 다룬 주요 논문을 아래에 정리했습니다. (PubMed 중심으로 검색)
- The impact of vitreous floaters on quality of life: a qualitative study (2025 Aug, J Patient Rep Outcomes) - 44명 환자 인터뷰 기반. 유병률 87% 언급, 삶의 질 영향(시각 증상, 불편, 감정적 고통) 강조. 예후: 만성적이지만 적응 가능, 치료 위험 논의.
- RWC Update: Pars Plana Vitrectomy for Symptomatic Vitreous Floaters (2025 Oct, Retina) - 증상성 비문증 수술 결과: 90-95% 주관적 개선. 예후: 대비 민감도 향상, 하지만 위험(감염, 망막 박리) 있음.
- Vision degrading myodesopsia from vitreous floaters in the young (2024, Surv Ophthalmol) - 젊은 근시 환자 중심 리뷰. 유병률: 근시 증가와 비례. 병기: 유리체 변화 과정 설명. 예후: 삶의 질 영향 크지만, 치료 옵션(레이저, 수술) 논의.
- Symptomatic Vitreous Opacities: Exploring the Mismatch between Clinical Observation and Self-Reported Symptoms (2024 Oct, J Clin Med) - 젊은 환자 증상 vs. 임상 소견 불일치 분석. 예후: 주관적 증상 강하지만, 객관적 변화 적음.
- Patient-reported outcomes in patients with vitreous floaters (2023, Surv Ophthalmol) - 환자 보고 결과 측정 도구 리뷰. 삶의 질 영향 강조, 유병률 및 예후 관련 PROMs 부족 지적.

방법
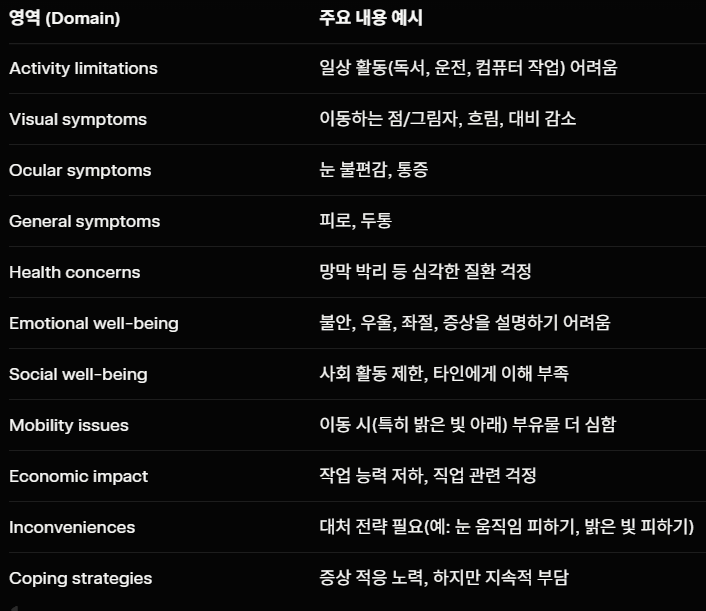 특히 강조된 점:
|

https://pubmed.ncbi.nlm.nih.gov/39424075/
| 비문증(유리체 부유물, vitreous floaters)은 눈 속 부유하는 불투명물로 인해 발생하는 시각 현상으로, 콜라겐 섬유가 응집되어 불규칙한(때때로 벌레 모양) 그림자나 구조물로 보입니다. 이는 투명~검은색으로 나타나며, 눈 움직임에 따라 따라 움직여 시야를 방해합니다. 이로 인해 대비 민감도(contrast sensitivity) 저하와 삶의 질(quality of life) 악화를 초래하는데, 이를 **vision degrading myodesopsia (VDM, 시야 저하성 근시안증)**라고 부릅니다. 전통적으로 비문증은 "무해한(harmless)" 것으로 여겨졌으나, 최근 삶의 질 영향이 주목받고 있습니다. 특히 젊은 층에서 VDM이 증가하고 있으며, 이는 근시(myopia) 유병률 증가와 밀접 관련이 있습니다. 근시성 유리체병증(myopic vitreopathy)이 젊은 환자의 주요 원인인데, 이 측면은 종종 간과됩니다. 주요 내용 (리뷰 범위) 이 논문은 젊은 근시 환자 관점에서 다음 주제를 종합 검토합니다:
|

| 젊은 환자에서 **증상성 유리체 혼탁(Symptomatic Vitreous Opacities, SVO)**으로 인한 주관적 증상과 임상적 유리체 변화 관찰 사이의 **불일치(mismatch)**를 평가하는 것. 특히, 건강한 젊은 층에서 비문증이 심각한데도 슬릿램프 검사에서 유리체가 정상처럼 보이는 이유를 탐색. 방법
|

| 비문증(유리체 부유물, vitreous floaters)이 환자의 삶의 질에 미치는 영향을 측정하고 치료 효과를 평가하기 위해 **환자보고 결과물(Patient-Reported Outcome Measures, PROMs)**이 필수적입니다. 이 논문은 비문증 환자를 대상으로 PROM을 사용한 모든 연구를 체계적으로 검토하여, 기존 PROM의 내용 범위, 개발 과정, 심리측정학적 품질(psychometric quality)을 평가합니다. 방법
|
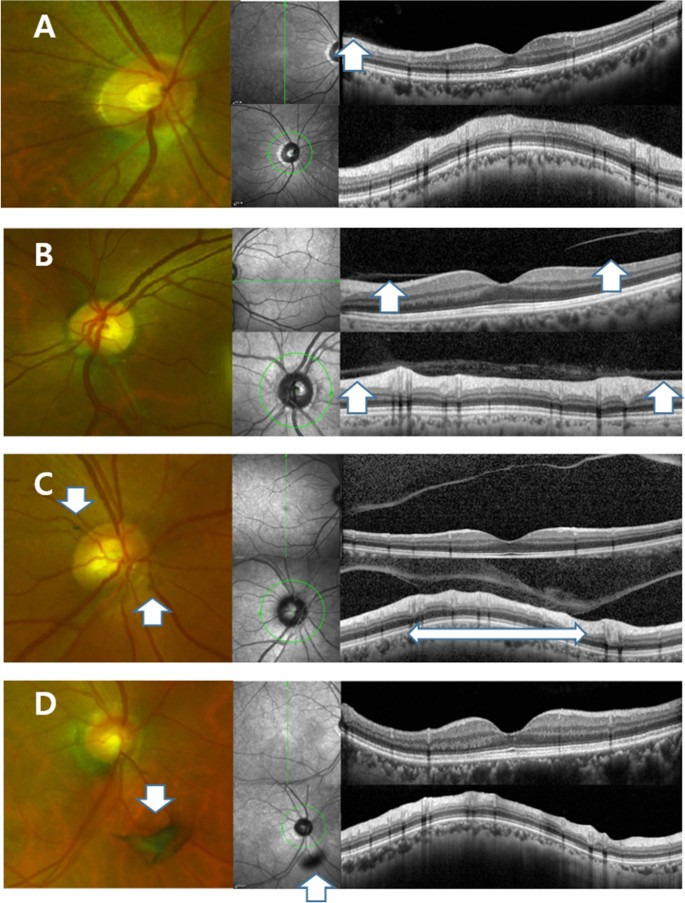
PVD 병기 분류 (OCT 기반, Itakura/Kishi classification)
|
- nature
- scientific reports
- articles
- article
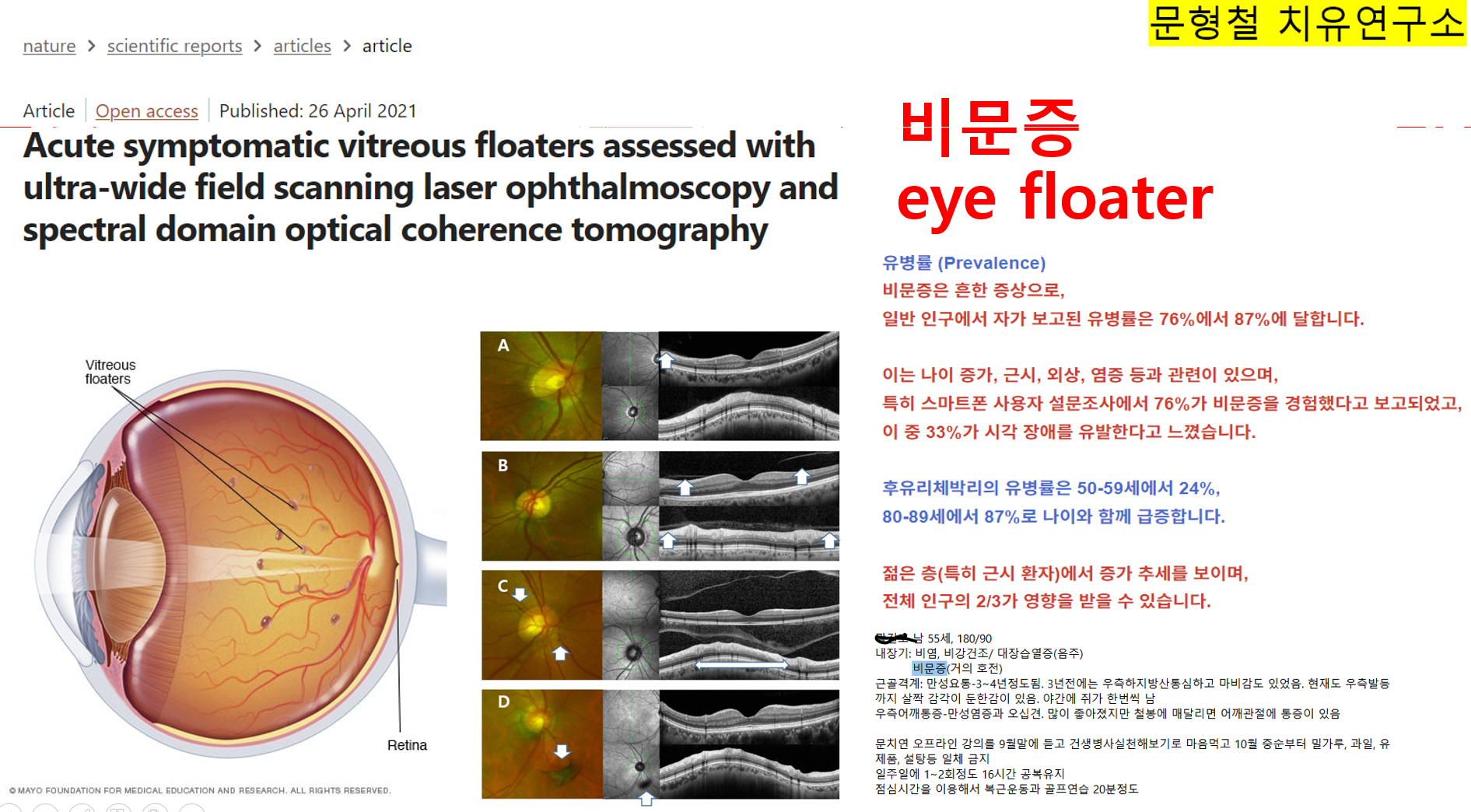
Acute symptomatic vitreous floaters assessed with ultra-wide field scanning laser ophthalmoscopy and spectral domain optical coherence tomography
- Article
- Open access
- Published: 26 April 2021
Acute symptomatic vitreous floaters assessed with ultra-wide field scanning laser ophthalmoscopy and spectral domain optical coherence tomography
Scientific Reports volume 11, Article number: 8930 (2021) Cite this article
Abstract
To describe the eyes with vitreous floaters and to analyze the development of acute symptomatic posterior vitreous detachment (PVD). A retrospective review of medical records was performed on patients with the vitreous floater developed for the first time of their life. Peripapillary vitreous opacity (pVO) was searched in Ultra-wide field (UWF) scanning laser ophthalmoscopy and PVD stage was assessed through spectral-domain optical coherence tomography (SD-OCT). 196 patients (55 males and 141 females), who were 58.4 (± 9.1) years old, visited a retinal clinic 9.4 (± 9.1) days after they experienced vitreous floaters. In 196 eyes, pVO was noticed in 122 eyes (62.2%) at UWF. In 106 eyes where SD-OCT data were available, PVD was noticed in 100 eyes (94.3%). Symptomatic eyes showed more advanced stage of PVD (p < 0.001) than symptom free eyes. Eyes with floaters were more myopic (− 0.7 ± 2.2D vs − 0.5 ± 1.9D, p = 0.02), and had lower intraocular pressure (IOP) (14.7 ± 3.2 mmHg vs 15.2 ± 3.0 mmHg, p = 0.02) than the other symptom free eyes. In patients with first floater symptoms, PVD was in progress in most of the eyes not only the symptomatic eyes but also on the contralateral symptom free eyes. Eyes with vitreous floaters were more myopic and had lower IOP than the opposite symptom free eyes.
유리체 부유물이 있는 눈을 기술하고 급성 증상성 후부 유리체 박리(PVD)의 진행을 분석하기 위함이다. 생애 처음으로 유리체 부유물이 발생한 환자들의 진료 기록을 후향적으로 검토하였다. 초광각(UWF) 스캐닝 레이저 안저경 검사로 시신경유두주위 유리체 혼탁(pVO)을 확인하고, 스펙트럼 도메인 광간섭 단층촬영(SD-OCT)을 통해 PVD 단계를 평가하였다.
유리체 부유물을 경험한 지 9.4일(±9.1) 후에
망막 클리닉을 방문한 196명의 환자(남성 55명, 여성 141명)의 평균 연령은 58.4세(±9.1)였다.
196안 중 UWF에서 pVO가 122안(62.2%)에서 관찰되었다.
SD-OCT 데이터가 확보된 106안 중 PVD는 100안(94.3%)에서 확인되었다.
증상이 있는 안은 증상이 없는 안보다 PVD 진행 단계가 더 심했다(p<0.001).
유리체 부유물이 있는 안구는
증상이 없는 다른 안구보다 근시가 더 심했으며(-0.7±2.2D vs -0.5±1.9D, p=0.02),
안압(IOP)도 더 낮았다(14.7±3.2 mmHg vs 15.2±3.0 mmHg, p=0.02).
첫 유목 증상이 나타난 환자에서, 증상이 있는 눈뿐만 아니라 반대쪽 증상이 없는 눈에서도 대부분의 눈에 유리체후막박리가 진행 중이었다. 유리체 유목이 있는 눈은 반대쪽 증상이 없는 눈보다 근시가 더 심하고 안압이 더 낮았다.
Similar content being viewed by others
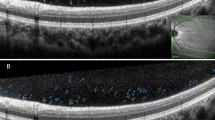
Punctate hyperreflective vitreous opacities: a ubiquitous finding in healthy children beyond infancy
Article 31 October 2024
Article Open access30 August 2021
Progression of posterior vitreous detachment after cataract surgery
Article 30 August 2021
Introduction
Vitreous floaters are entoptic images of opacity in vitreous cavity1. Substantial portion of patients visit retina clinics complaining symptomatic degenerative floaters. Although floater symptoms often become asymptomatic within a few months from onset, they do cause visual discomfort such as blurred vision, glare and haze in daily living for months or years2. Moreover, degenerative vitreous floaters related with posterior vitreous detachment (PVD) could be more clinically significant because they can be followed by pathologic conditions such as vitreous hemorrhage, retinal tear or retinal detachment3. Therefore, characterizing the status of PVD could provide important information on eyes with acute vitreous floaters.
Recently, detailed evaluation of vitreoretinal interface has been possible since the introduction of spectral domain optical coherence tomography (SD-OCT)4,5,6,7,8. And ultra-wide field retinal imaging (UWF) devices allow us to evaluate posterior pole and wide range of the peripheral retina simultaneously9. We hypothesized that the SD-OCT and UWF examination will allow us to identify and record PVD status more accurately. Thus, we investigated patients with acute symptomatic vitreous floaters using these two modalities to determine the relationship between floaters and PVD. By comparing eyes with and without floater symptoms, we also intended to find out when floater symptoms occur on the process of PVD.
서론
유리체 부유물은
유리체강 내 혼탁물의 내시경적 영상이다1.
상당수 환자들이 증상이 있는 퇴행성 부유물을 호소하며 망막 클리닉을 방문한다.
부유물 증상은 발병 후 몇 개월 내에 무증상화되는 경우가 많지만,
수개월 또는 수년간 일상생활에서
시야 흐림, 눈부심, 안개 현상 등의 시각적 불편감을 유발한다2.
또한 후부 유리체 박리(PVD)와 관련된 퇴행성 유리체 부유물은
유리체 출혈, 망막열상 또는 망막박리3과 같은 병리적 상태를 동반할 수 있어 임상적으로 더 중요할 수 있습니다.
따라서
PVD 상태를 특성화하는 것은 급성 유리체 부유물이 있는 눈에 대한 중요한 정보를 제공할 수 있습니다.
최근 스펙트럼 도메인 광학 코히런스 단층촬영(SD-OCT)의 도입으로 유리체망막 접합부의 상세한 평가가 가능해졌다4,5,6,7,8. 또한 초광각 망막 촬영(UWF) 장치는 후극부와 광범위한 주변 망막을 동시에 평가할 수 있게 한다9. 우리는 SD-OCT와 UWF 검사를 통해 유리체후박리 상태를 보다 정확하게 확인하고 기록할 수 있을 것이라는 가설을 세웠다. 이에 유리체후박리와 유동체 증상 간의 관계를 규명하기 위해 이 두 가지 검사를 활용하여 급성 증상성 유리체 유동체 환자를 조사하였다. 또한 유동체 증상이 있는 눈과 없는 눈을 비교함으로써 유리체후박리 진행 과정에서 유동체 증상이 언제 발생하는지 알아내고자 하였다.
Results
The mean age was 58.38 (± 9.14) years old in average, consisting of 141 women and 55 men (Table 1). The BCVA of 196 eyes was 0.06 (± 0.10) in average, SE was − 0.70 (± 2.09) diopter, and intraocular pressure (IOP) was 15.05 (± 6.20) mmHg. There was no difference between men and women in BCVA (p = 0.64), SE (p = 0.45) and IOP (p = 0.11). In 33 patients (17.3%), vitreous floaters were found in both eyes. Patients visited our retina clinic after an average of 9.41 (± 9.05) days after symptom onset, and 23 patients (11.74%) had ‘flashing light’ symptom before the floater. 24 patients (12.24%) needed laser treatment on peripheral retinal break which was observed in their clinical visit. In 3 eyes (1.53%), glaucoma was diagnosed incidentally and those 3 eyes were excluded from the pRNFL analysis.
Table 1 Demographics and ophthalmological outcomes of eyes with acute subjective vitreous floaters occurred within 1 month.
Of the 196 eyes with floater, 97 eyes (49.5%) were emmetropic (− 1D < SE < + 1D), 61 eyes (31.1%) were myopic (SE ≤ − 1D) and 38 eyes (19.4%) were hyperopic (SE ≥ + 1D). Myopic eyes tend to present vitreous floater symptoms earlier (r = 0.406, p < 0.001, Fig. 1). This was the same for both the male group (r = 0.352, p = 0.008) and the female group (r = 0.463, p < 0.001). In addition, thinner pRNFL was observed in Myopic patients (r = 0.299, p = 0.011), and SE was not significantly related to central macular thickness (CMT) (r = 0.072, p = 0.471).
Figure 1
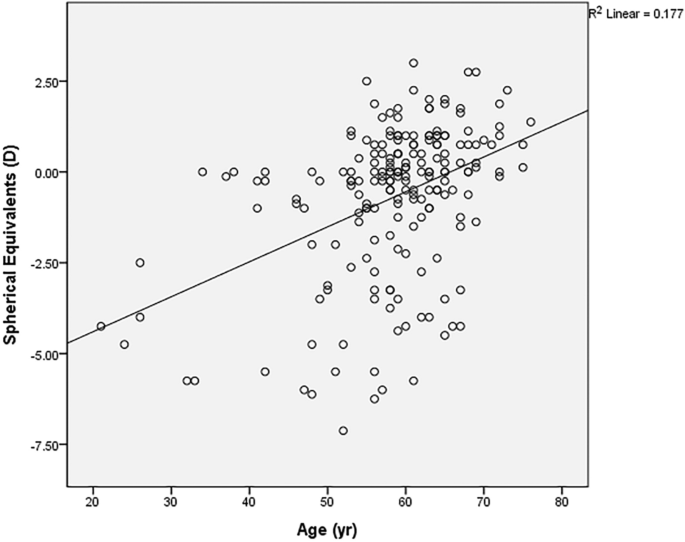
X-axis presents the age when the first vitreous floater symptom occurred, while Y-axis presents the spherical equivalent value in diopters (D). The oblique line of best fit is showing a positive correlation between the spherical equivalent value and age. (r = 0.421, p < 0.001 in the Pearson’s correlation analysis).
Peripapillary vitreous opacity (pVO) was observed in 62.2% (122 out of 196 eyes) in the UWF image. Among 106 symptomatic eyes where SD-OCT data were available, PVD was identified in 94.3% on SD-OCT. PVD was staged based on the morphology of the vitreomacular interphase assessed with SD-OCT, from stage 0 to 4. In 106 symptomatic eyes, 6 eyes were categorized as stage 0, while 8 eyes as stage 1, 6 eyes as stage 2, 5 eyes as stage 3 and 81 eyes as stage 4. Interestingly, almost every eye with the pVO had the evidence of PVD on SD-OCT (98.7%, 75 out of 76 eyes). While, 75.0% (75 eyes out of 100 eyes) of eyes with SD-OCT proven PVD had pVO on UWF images.
We compared the ophthalmologic examination results of the symptomatic study eyes with floaters and the symptom free contralateral eyes without floaters in 163 patients who had symptoms only in the unilateral eye (Table 2). The eyes with floaters were more myopic than those without floaters (− 0.7 ± 2.2D vs − 0.5 ± 1.9D, p = 0.02), and had lower intraocular pressure (14.7 ± 3.2 mmHg vs 15.2 ± 3.0 mmHg, p = 0.02). Visual acuity (0.06 ± 0.11 vs 0.04 ± 0.08, p = 0.09), CMT (259.4 ± 20.2 vs 260.0 ± 19.5, p = 0.56) or pRNFL (100.7 ± 11.6 μm vs 100.5 ± 11.4 μm, p = 0.08) did not differ between the two groups. More pVO on UWF (63.2% vs 18.4%, p = 0.04) and more advantaged PVD stage on SD-OCT (p < 0.001) was observed in the eyes with floater symptoms than the symptom free collateral eyes.
Table 2 Comparison between ophthalmological outcomes of eyes with and without vitreous floaters among patients with unilateral symptomatic eyes.
We could verify a high degree of agreement on the interpretation of UWF and SD-OCT images between two investigators (GSS, MGK) In UWF image analyses, the judgments were in agreement in 190 eyes (96.9%). Regarding SD-OCT image analyses, the ICC value between the two investigators was 0.977. There were six discordant interpretations on UWF images of myopic eyes with tessellated fundus. And there were three disagreements on SD-OCT images where background reflectivity of vitreous cavity was difficult to be determined as vitreous body or not.
Additional ophthalmological analyses were performed on 33 patients with floater symptoms on both eyes (Supplementary Table 1). The comparison was conducted between eyes with earlier floater symptoms versus eyes with more recently occurred floater symptoms. BCVA, SE, IOP, CMT and pRNFL thickness were not different each other (p = 0.48, 0.39, 0.24, 0.65, 0.71 respectively). The prevalence of the pVO on the UWF were not different between 2 groups, (57.6% vs 36.4, p = 0.505) neither so PVD stage (p = 0.90).
Discussion
This study provides novel information regarding the vitreoretinal interface of patients experiencing their lifetime’s first floater symptom. Meanwhile, through this study, we were able to confirm several facts that have been reported about PVD in previous studies. First, the first vitreous floater in life showed at an average age of 58.4 years, similar to the previous studies10,11,12,13. The female predominance of PVD in this study (72% in female) has been also reported several times in previous studies10,13. In addition, the earlier onset of PVD in the myopic eye in this study has also been reported in several other previous studies10,14,15.
The usefulness of SD-OCT in the diagnosis of PVD was recently presented in a previous prospective study. Moon et al.16 analyzed 124 eyes with PVD examined using ultrasonography and SD-OCT and showed the usefulness of adding peripapillary OCT scans in the diagnosis of PVD considering lower inter-examiner agreement of ocular ultrasound scanning. Our data could be convincing evidences supporting their hypothesis. Instead of ultrasonography, however, we described the inter-correlation of UWF and SD-OCT assessing eyes with vitreous floaters. We believe that our study could describe more ‘real world’ clinical situation than their data analyzed from prospectively enrolled patients.
Most of the eyes with floaters had PVD in progress, and the proportion was 94.3% as determined by the SD-OCT. Interestingly, PVD was also progressing in most of the asymptomatic eyes. We confirmed the evidence of PVD assessed with SD-OCT in 89.5% of the symptom free contralateral eyes. This inconsistency between presence of PVD on SD-OCT and absence of subjective symptoms could be explained by the PVD stage of the opposite symptom free eye which was earlier than the other symptomatic eye. In other words, the degree of detached membrane might be relatively small to be noticed in earlier PVD stage. Since this study is cross sectional, it was difficult to accurately determine at which point the floater occurred during the PVD process. However, we could confirm that the eyes with floater present more advanced PVD stage on SD-OCT and more eyes with pVO on UWF than the symptom free contralateral eyes.
The fact that the eyes with floaters were more myopic and had lower IOP can be explained in relation to changes in the eyeball as PVD progresses. Myopic eyes have longer axial length, so maybe easily affected by the shrinkage of the vitreous body. We can also infer that a more myopic eye in a single person might expect earlier vitreous floaters than the other eye. Meanwhile, the measurement of low intraocular pressure in PVD eyes can be explained by the fact that stiffer vitreous in eyes without PVD may present a stronger rebound than liquefied vitreous in eyes with PVD during the measurement of IOP.
Peripapillary vitreous opacity presented on UWF could be thought as a convincing evidence of PVD. This can be intuitively understood, because the pVO is likely to be found in UWF after PVD initiation. Weiss ring, which is the representative form of pVO in the advanced stage PVD, is noticed when complete PVD occurs after the detachment of the vitreopapillary adhesion. Also in this study, almost every eyes with visible pVO were proven to have PVD through SD-OCT examination. For a few exceptional cases (2 eyes, 2.67%), pVO could be positioned perpendicular to the front, difficult to be photographed. Considering this, if Weiss ring is observed in UWF, ophthalmologists who are practicing in the environment without SD-OCT equipment could be more confident in the presence of the PVD.
Based on this study results, retinal examinations of both eyes are recommendable on the patients complaining of floaters. This is because described above, PVD was occurring in 89.5% of the contralateral eyes even without subjective floater symptoms. If early-staged PVD findings on SD-OCT are observed in the opposite eye, the patient can be explained in advance that floater symptoms may also occur in the symptom free eyes. In addition, in 6 eyes (1.95%) of the study cohort, a peripheral retinal break requiring laser photocoagulation treatment was found in the opposite eye rather than in the symptomatic eye.
Despite high degree of agreement, discrepancy in the interpretation of UWF and SD-OCT tests between the two investigators should not be ignored. In 6 UWF images, there was a disagreement whether the spots on the photos to be judged by vitreous opacity or peripapillary pigments. The ambiguity got bigger in myopic eyes with tessellated fundus. In 3 SD-OCT images, it was difficult to determine whether PVD stage be categorized into stage 1 or stage 2. Serial checks-up of the test, correlations with the stereoscopic fundus examination findings or performing swept-source OCT covering more extensive retina could be helpful approaches for solving the discrepancy.
Although it is useful to examine UWF and SD-OCT together in patients with vitreous floaters, yet detailed medical history and meticulous retinal observation through a microscope should not be overlooked. This is because floater symptoms are not necessarily caused by PVD. If we listen to the patients carefully through detailed medical history, we can better understand the patients-reporting ‘floaters’ symptoms. Thorough retinal examination should be performed to conclude whether vitreous opacities are related with PVD or not.
We are mindful of the limitations of this study, such as its retrospective and cross-sectional nature performed on single-ethnic population background. In addition, section bias should be mentioned as we analyzed only the patients who visited clinic. In addition, SD-OCT was performed on 106 patients (53%) who were willing to pay for the examination. However, as we know of, this is the first attempt to analyze lifetime’s first vitreous floaters using both of the UWF scanning laser ophthalmoscopy and the SD-OCT images. We believe our study might provide useful information to ophthalmologists regarding vitreous floaters and PVD in real clinical world. Further prospective studies might warrant for more useful information of when and in what percent the vitreous floater symptoms fades away.
Methods
We retrospectively analyzed the medical records of patients who visited our retina clinic due to newly developed vitreous floaters within a month from July 2017 to May 2020. All patients received thorough ophthalmological examination including BCVA, manifest refraction, IOP (NT-530P, Nidek, Aichi, Japan), retinal examination after mydriasis, SD-OCT (Version 5.3.2.0; Heidelberg Engineering, Heidelberg, Germany) and UWF (Optomap, Optos PLC, Dunfermline, Fife, Scotland, UK) were performed. We conducted SD-OCT line and raster scan in all eyes centered at the fovea. Automatic real-time (ART) mode was activated when horizontal and vertical line scans were conducted with 25 frames averaged. In the raster scan image, a 30 × 25 degree2 area was covered with 31 b-scans (consisting of 768 A-scans), which are 9.0 mm in length, and spaced at 240 μm apart. The peripapillary region was scanned using a circular scan 12° in diameter, centered on the optic disc (Fig. 2). Every retinal examination was performed on both eyes. All the images information was assessed by saved data on digital files before in-depth analyses.
Figure 2
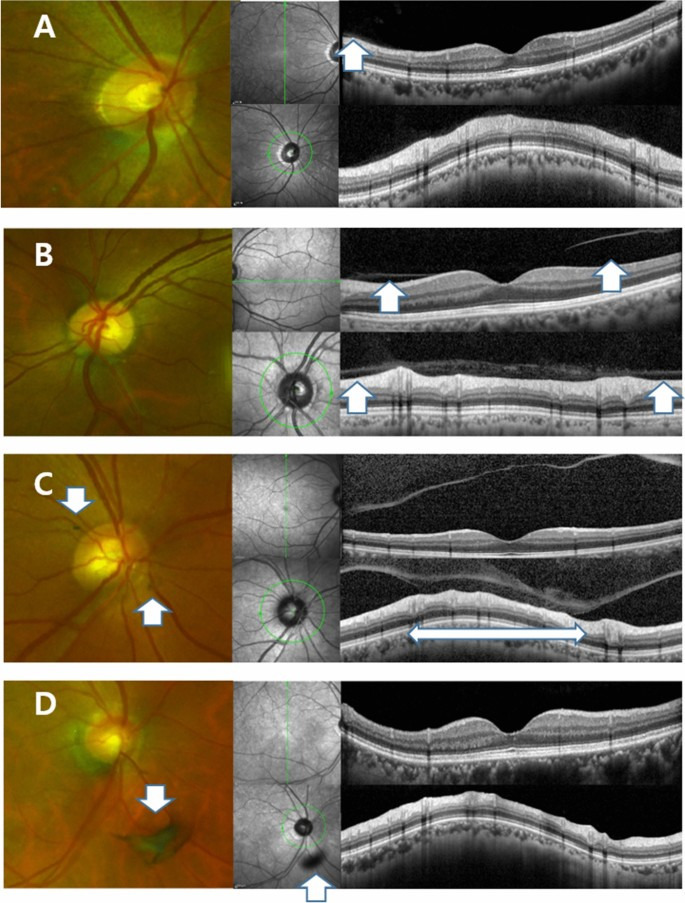
Ultra-wide field scanning laser ophthalmoscopy (UWF) and Spectral Domain Optical Coherence Tomography (SD-OCT) images of patients who experienced floater for the first time in their life. (A) PVD stage 1. 59 year-old male. No definite change was noticed around optic disc in UWF. Note subtle change which is presenting the initiation of PVD (Posterior Vitreous Detachment, white arrow). (B) PVD stage 2. 60 year-old female. No definite change was noticed around optic disc in UWF. In the macular SD-OCT image, perifoveal posterior vitreous detachment (PVD) is in progress (white arrows) remaining posterior vitreous attached to fovea. In glaucomatous SD-OCT, PVD is in progress in some part of the optic disc margin (arrow), while most of the optic disc remains attached to the vitreous body. (C) PVD stage 3. 61 year-old male. Note two pVOs (peripapillary vitreous opacity, white arrows) noticed around the optic disc. In the macular SD-OCT image, PVD occurred throughout the entire macula. In the glaucomatous SD-OCT image, PVD is in progress while about half of the optic disc margin is detached to the vitreous body (a wide bidirectional arrow). (D) PVD stage 4. 66 year-old female. Note a dense pVO (white arrow) resembling a Weiss ring. In the macular SD-OCT image, reflectivity of vitreous body is not observed in hollow vitreous cavity. In glaucomatous SD-OCT image, reflectivity of vitreous body is not observed either. A shadow of pVO (arrow) is identified.
Study subjects and vitreous floaters
Eligible subjects were adults older than 20 years old who experienced acute symptom (onset ≤ 1 month) of vitreous floaters for the first time of their life. In patients with floater symptoms in both eyes, eyes with more recently developed floater symptom were selected for the analysis. Exclusion criteria includes history of ocular surgery including cataract operation, history of ocular injections, any retinopathy including diabetic retinopathy or retinal vein occlusion, medial opacity including severe cataract or corneal opacity or eyes with obscure image which were not suitable for proper analyses. Eyes received refractive surgeries were excluded from the refraction analyses.
In this study, vitreous floaters were defined as symptoms of unprecedented amorphous ‘floating’ material. Other confusing symptoms such as fixed spots interrupts visual axis, transient wavy visual disturbance or metamorphopsia were excluded with through history taking. Concurrent subjective symptoms such as headaches, flashes, or ocular pain were asked also.
Analyses of ophthalmologic outcomes
Best-corrected visual acuity was measured with the manifest refraction test and was recorded in logMAR (logarithm of minimal angle of resolution). The spherical equivalent and cylindrical value were expressed in diopter. CMT at the 1-mm center of the fovea was measured using a built-in software (Heidelberg Eye Explorer, version 1.10.2.0, Heidelberg Engineering, Heidelberg, Germany), which recorded the distance between the vitreoretinal surface and the border between the retinal pigment epithelium and the Bruch’s membrane. Peripapillary RNFL (pRNFL) thickness was measured using the identical software.
Analysis of peripapillary vitreous opacity in UWF imaging
The presence of pVO was observed in UWF images taken on the eyes, after pupil dilation. The vitreous opacity found within 3 disc diameters from the center of the disc was included (Fig. 2). In cases where it was difficult to judge by pictures alone, the precise fundus examination with indirect ophthalmoscopy was considered together for the determination. The two investigators (GSS, MK) each independently analyzed the image, and for the inconsistencies, the senior investigator (JHS) made a final decision.
Anaylsis of PVD stage in SD-OCT imaging
The staging of PVD was performed base on the previously published paper17. In brief, stage 0 = no PVD; stage 1 = PVD at mid-periphery and possible subtle PVD in the posterior retina; stage 2 = PVD, except for persistent adhesion to the papilla and fovea; stage 3 = PVD, except for persistent adhesion to the papilla; and Stage 4 = complete PVD (Fig. 2). The two investigators (GSS, MK) analyzed PVD respectively, and the opinions of senior investigator (JHS) were sought for discordant findings.
Statistical analyses
Continuous values were expressed as “average ± standard deviation,” and categorical variables were described as proportions; differences between groups were determined using the Chi-squared test or Fisher’s exact test. Comparison of ophthalmological values between eyes with/without vitreous floaters was performed using the paired t test. Pearson’s correlation analyses were performed among various continuous values. Inter-class correlation (ICC) value was calculated to determine how consistent the two investigators’ interpretations on PVD at SD-OCT images were. All data were inserted into an Excel spreadsheet (Microsoft Corp.) and analyzed using SPSS software (version 23; IBM Corp, New York, NY). A P-value less than 0.05 was considered statistically significant.
Ethics approval and patient consent
This study was approved by the Institutional Review Board (IRB) of Hangil Eye Hospital (IRB number: IRB-20006) and complied with the Declaration of Helsinki in conducting the study. Given the retrospective design of this study and the use of anonymized data, requirements for informed consent were waived by the IRB.
References

